|
The Well Being of Our Nation:
An Inter-Generational Vision of Effective Mental
Health Services and Supports
National Council on Disability
September 16,
2002
National Council on Disability
1331 F Street, NW, Suite
850
Washington, DC 20004
The Well Being of our Nation: An Inter-Generational Vision of
Effective Mental Health Services and Supports
This report is also available in alternative formats and on NCD's
award-winning Web site (http://www.ncd.gov/newsroom/publications/(http://www.ncd.gov).).
Publication date: September 16, 2002
202-272-2004 Voice
202-272-2074 TTY
202-272-2022 Fax
The views contained in the report do not necessarily represent those of
the Administration as this and all NCD documents are not subject to the
A-19 Executive Branch review process.
National Council on Disability
Members and Staff
Members
Lex Frieden, Chairperson
Kate Pew
Wolters, First Vice Chairperson
Hughey Walker, Second Vice
Chairperson
Yerker Andersson, Ph.D.
Dave N. Brown
Robert R.
Davila, Ph.D.
Young Woo Kang, Ph.D.
Kathleen Martinez
Audrey
McCrimon
Carol Hughes Novak
Bonnie O'Day, Ph.D.
Patricia
Pound
Lilliam Rangel-Diaz
Staff
Ethel D. Briggs, Executive
Director
Jeffrey T. Rosen, General Counsel and Director of
Policy
Mark S. Quigley, Director of Communications
Allan W. Holland,
Chief Financial Officer
Julie H. Carroll, Attorney Advisor
Joan M.
Durocher, Attorney Advisor
Martin Gould, Ed.D., Senior Research
Specialist
Gerrie Drake Hawkins, Ph.D., Program Specialist
Pamela
O'Leary, Interpreter
Brenda Bratton, Executive Assistant
Stacey S.
Brown, Staff Assistant
Carla Nelson, Office Automation Clerk
Acknowledgment
The policy research and analysis was conducted, and a report to the
National Council on Disability (NCD) prepared, through a contract with
Michael Allen and the Bazelon Center for Mental Health Law. Michael Allen
is a lawyer, a policy researcher, and a seasoned writer in the area of
mental health services.
Contents
Executive
Summary
Chapter
1: Introduction
Chapter
2: How Did We Get Here?
Chapter
3: Impact on Children and Youth
Chapter
4: Impact on Adults
Chapter
5: Impact on Seniors
Chapter
6: Fulfilling the Promise: Concrete Steps Toward a New Vision
Chapter
7: An Inter-Generational Vision for Effective Mental Health Services and
Supports
Appendix
Mission
of the National Council on Disability
Executive Summary
At a time when more is known about mental illnesses than at any other
time in history and just three years after the U.S. Supreme Court held
that unnecessary institutionalization violates the Americans with
Disabilities Act, public mental health systems find themselves in crisis,
unable to provide even the most basic mental health services and supports
to help people with psychiatric disabilities become full members of the
communities in which they live.
This report does not aim to be a comprehensive review of all that is
known about public mental health and its shortcomings. That undertaking
has been begun by the U.S. Surgeon General, in the massive 1999 report
entitled Mental Health: A Report of the Surgeon General (http://www.surgeongeneral.gov/library/mentalhealth/home.html),
and will be carried on with President Bush's New Freedom Commission on
Mental Health, which held its first public hearings in July 2002. Rather,
this report examines some of the root causes of the crisis in mental
health, and seeks to "connect the dots" concerning the dysfunction of a
number of public systems that are charged with providing mental health
services and supports for children, youth, adults and seniors who have
been diagnosed with mental illnesses.
One of the most significant findings of this report is that children
and youth who experience dysfunction at the hands of mental health and
educational systems are much more likely to become dependent on failing
systems that are supposed to serve adults. In parallel fashion, adults
whose mental health service and support needs are not fulfilled are very
likely to become seniors who are dependent on failing public systems of
care. In this fashion, hundreds of thousands of children, youth, adults
and seniors experience poor services and poor life outcomes, literally
from cradle to grave.
There is no single antidote for the current dysfunction of the public
mental health system. Clearly, visionary leadership, adequate funding and
expansion of proven models (including consumer-directed programs) are
essential ingredients. More than these, however, there needs to be a
dramatic shift in aspirations for people with psychiatric disabilities.
Public mental health systems must be driven by a value system that sees
recovery as achievable and desirable for every person who has experienced
mental illness. Systems also must commit to serving the whole person, and
not merely the most obvious symptoms. In other words, mental health
systems will have to develop the expertise to deliver not just medication
and counseling, but housing, transportation and employment supports as
well.
There are proven models of success throughout the country, but
entrenched forces and stale thinking have prevented them from "going to
scale" to serve more people with psychiatric disabilities. Some such
models are referenced throughout the report, and Chapter 6 provides a menu
of concrete actions to bring about a new vision of public mental health
services and supports.
Chapter 1
Introduction
For decades, state mental health systems have been burdened with
ineffective service-delivery programs and stagnant bureaucracies. Their
operations have become rote, spurred to change only by crises. Combined
with ever-increasing fiscal pressures, this situation has precluded
innovation and kept most systems from incorporating the new and more
effective interventions developed in recent years. As a result, state
mental health systems have all but disintegrated, falling ever farther
from the ideal of voluntary, accessible and effective services and
supports that promote meaningful community membership.
As large state psychiatric hospitals have been downsized or closed over
the past 30 years, people with psychiatric disabilities, advocates,
providers and policy makers have learned that recovery from mental illness
requires much more than traditional "mental health services." Rather,
recovery may require access to housing, transportation, employment and
peer supports and, for certain individuals, these may be much more
important than medication, therapy and case management. Yet, with rare
exceptions,1
mental health systems have been slow to acknowledge and respond to these
needs with meaningful, naturalistic supports. Throughout this report,
reference will be made to "mental health services and supports" to
highlight the critical importance of each in providing the tools that a
person with a psychiatric disability may need to recover from symptoms of
mental illness, to overcome isolation and to gain (or regain) economic
self-sufficiency.
A growing number of advocates, policymakers and members of the media
have begun to realize that the public mental health system
(2)
in most states is highly dysfunctional, and rations care in a manner
that requires people with serious mental illnesses to "hit bottom" before
receiving the services and supports they need to live successfully in the
community
(3)
. The depressing reality is that this approach is shared by systems
serving children, youth, adults and seniors, creating dependency and
perpetuating failure, sometimes literally from cradle to grave.
In fact, the use of the term "mental health system" is, itself,
problematic. One of the primary problems is that states do not have a
single system of mental health care, but a number of patchwork systems
that are called upon to provide such care, often without a guiding vision
of how to do so most effectively and frequently without the funding to
actually deliver services and support to every eligible person. To be
diagnosed with a mental illness (or with "severe emotional distress," the
term applied to children and youth under the age of 18) is to be consigned
to one dysfunctional system after another. In fact, the evidence shows
that once the label has been applied and a person has been failed by one
public system, chances are high that he or she will frequently be failed
by other systems as well.
Throughout the 1970s, 1980s, and 1990s, whether in times of budgetary
deficit or surplus, states failed to adequately fund their mental health
systems. But the pressing needs of people with mental illnesses did not
just disappear. They were forced underground or, more accurately, they
were forced onto other public and private systems that were not designed
to provide mental health services and supports.
In many communities, jails and prisons become the safety nets and the
largest providers of mental health services. Homeless shelters and nursing
homes have become housing of last resort for people with mental illnesses.
Hospital emergency rooms have provided crisis-oriented care for a few days
at a time before sending people with mental illnesses back into a
community setting where they are destined to fail because of a lack of
mental health services and supports.
When children and youth with severe emotional disturbance cannot get
the family-based care and supports they need, they often end up in foster
care or juvenile justice, and may be consigned to institutional settings
where they are further cut off from their natural support systems. Seniors
with unmet mental health needs are often relegated to nursing homes or
unregulated "board and care" homes where they are left to fend for
themselves.
While they do not appear on the budget line for the state mental health
agency, the costs of care for people with mental illnesses are borne by
these other systems (and by taxpayers). Typically, these costs are many
times higher than what it would cost to provide modest, preventive
services and supports, such as counseling, peer support, respite care,
supportive housing and job training.
Beyond funding, one of the most significant barriers to access is that,
outside of psychiatric hospitals, the public mental health system is only
"open" from 9 a.m. to 5 p.m. By contrast, law enforcement, jails and
prisons, emergency rooms, homeless shelters and other systems are "open"
24/7 and, as a consequence, have ended up taking a larger share of people
in crisis.
Through neglect or underfunding, the public mental health system in
many states has effectively closed its doors, through the use of waiting
lists, priorities for service, and disqualification of people who are
thought to be "hard to serve" or "treatment resistant." As a consequence,
adults with mental illnesses have increasingly found themselves caught up
with law enforcement, the judicial system and the correctional system.
(4)
Children and youth with severe emotional disturbance are also shunted
from system to system, without adequate care from any of them. Even where
they have a legal entitlement to services-such as Medicaid's Early
Periodic Screening, Diagnosis and Treatment (EPSDT) program or the right
to a "free and appropriate public education" under the Individuals with
Disabilities Education Act (IDEA)--enforcement of these entitlements is
problematic because of a shortage of knowledgeable attorneys willing to
take on such claims.
When families can't enforce their children's right to services and
supports designed to keep them at home (or when they run out of private
insurance benefits), they are often forced to relinquish custody to the
state, which then provides fully-funded Medicaid services to secure
services very similar to those that had been denied to families, or had
been difficult for families to access.
As a result of all these shortcomings, people with psychiatric
disabilities, family members, advocates and members of the general public
have extremely low expectations of the mental health system, and even
these are often frustrated.
This paper is designed to provide a broad overview of the current state
of public systems charged with providing mental health services and
supports to children, youth, adults and seniors and to identify, across
these age groups, common trends that have led to the failure of these
public systems. It will do so by examining the following themes:
- Mental health systems are focused on crisis and on those "most in
need," requiring that people with psychiatric disabilities "hit bottom"
before getting the services and supports they need;
- Missed opportunities for prevention: The failure of community-based
and preventive systems leads to greater reliance on isolating
institutions and segregated "residential placements";
- Despite clear eligibility, many people are denied mental health
services and supports, or find them entirely inaccessible; and
- The failure to provide timely, voluntary and effective mental health
services and supports leads to tragic consequences for people with
psychiatric disabilities and for society at large.
Chapter 2
How Did We Get Here?
Since the early 1960s, national policy on serving people with serious
mental illnesses has focused on reducing costly and often neglectful
institutional care and relying, instead, on providing services more
humanely in the community. This movement acquired the unwieldy title of
"deinstitutionalization." One impetus in the early 1970s was the landmark
decision in the case of Wyatt v. Stickney,
(5)
which established a constitutional right for people confined in state
mental institutions to receive treatment for the condition that led to
their confinement, rather than being merely warehoused.
In the landmark Olmstead decision (Olmstead v. L.C., 119 S.Ct.
2176, 2188 (1999)), which reaffirmed the ADA's integration mandate, the
Supreme Court stated that "Unjustified segregation in an
institution...is properly regarded as discrimination based on
disability." Moreover, in her majority opinion, Judge Ruth
Bader-Ginsburg observed that: (a) "institutional placement of persons who
can handle and benefit from community settings perpetuates unwarranted
assumptions that persons so isolated are incapable or unworthy of
participating in community life," and (b) "confinement in an institution
severely diminishes the everyday life activities of individuals, including
family relations, social contacts, work options, economic independence,
educational advancement, and cultural enrichment." The decision makes
clear that the ingrained neglect of public systems constitutes a violation
of civil rights. It compels states to consider how their systems of care
perpetuate needless segregation and its harmful effects.
Despite many court orders and legislative pronouncements, however, the
ambitions of deinstitutionalization have yet to be realized. There is no
comprehensive community-based service systems that were deemed necessary
for people with psychiatric disabilities to thrive as they returned home.
Lacking access to the services and supports that promote self-sufficiency,
adults with serious mental illnesses such as schizophrenia, bipolar
disorder and major depression, and children and youth with emotional
disturbance remain vulnerable to homelessness, frequent
re-hospitalizations, unemployment and involvement with criminal justice
systems.
Access to Services Through Public Programs
People who either do not have private health insurance or exhaust their
coverage must turn to public-sector mental health programs. Unfortunately,
shrinking public-sector resources means that most of the uninsured are
unable to get the services and supports they need. They are given what is
available-often no more than a bimonthly appointment with a psychiatrist
and a supply of medication meant to suppress symptoms. In this fashion
most people with psychiatric disabilities who are poor are merely being
"warehoused" in the community rather than being helped toward recovery and
independence.
Federal Medicaid law requires that all covered children and youth have
access to all medically necessary services, through the Early and Periodic
Screening, Diagnosis, and Treatment (EPSDT) mandate. But many states do
not adequately implement EPSDT, nor do they require their managed care
contractors to do so.
(6)
Medicaid law prohibits reimbursement to psychiatric hospitals for
non-elderly adults. It does, however, permit states to cover a full array
of comprehensive community-based services. Yet many states have failed to
use these options, leaving some, particularly adults with serious mental
illness, without access to the array of effective services detailed in the
Surgeon General's report, such as targeted case management and psychiatric
rehabilitation, let alone help with housing, transportation and
employment.
Children, youth and adults with the most serious forms of mental
disability are victims of neglectful public systems that preclude their
access to the resources necessary for stable lives and meaningful
participation in the community. They are further victimized when the
consequences of unmet needs are punitive--for example, when they are
arrested for behavior, such as sleeping on the street, that is an outcome
of their lack of access to housing and mental health services.
Federal Mental Health Block Grant. The Federal Government,
through the Supreme Court's ruling in Olmstead has clarified the
duties of states to provide appropriate community services in lieu of
institutional care for people with mental illness. It would be
appropriate, at this time, for the Federal Government itself to increase
its financial contribution to spending on community mental health services
through the major mental health services program, the Community Mental
Health Services Block Grant.
(7)
Over the past 18 years, federal appropriations for the mental health
block grant have fallen in real terms. In 1980, community mental health
centers received $293 million in annual federal appropriations--a small
amount in overall mental health spending, but nonetheless an important
proportion of the resources available for community care. However, even
that modest amount looks significant today. In 1981, when the community
mental health law was repealed and the mental health block grant was
enacted to replace it, spending was reduced 14 percent. Following this
substantial cut, the block grant has continued to drastically lose ground
to inflation, as the graph below illustrates.
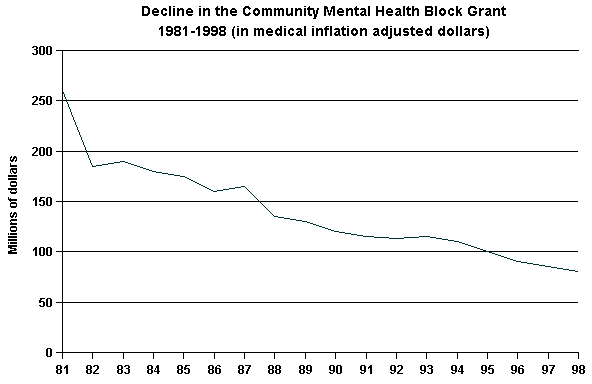 [D] [D]
(Source: Bazelon Center for Mental Health Law, Under Court Order:
What the Community Integration Mandate Means for People with Mental
Illnesses)
The Federal Government could, and should, do more to assist states in
meeting the needs of individuals who are unnecessarily institutionalized
or at risk of unnecessary institutionalization. In January 1999, the
administration requested that Congress increase appropriations for the
mental health block grant by $70 million. Such an increase, while helpful,
is far short of the level needed to restore lost spending power for the
block grant. Advocates should urge the administration and the Congress to
increase federal appropriations for the block grant to $1 billion. This
would raise spending on mental health to a level more commensurate with
spending under the substance abuse block grant ($1.585 billion).
Inadequate federal funding is exacerbating a crisis in community mental
health at the state and local levels, where budget shortfalls are leading
to drastic cuts in vital mental health programs. The landmark report on
mental health issued by the Surgeon General of the United States in
December 1999 affirmed that the technology exists to provide effective
treatment--even to people with serious mental illnesses. The problem is
that these treatments are simply not accessible to all who could benefit
from them.
State Appropriations
Community mental health services are generally no more expensive than
institutional care. However, to shift a system from over-reliance on
institutions to one that provides more appropriate and more effective
community services and supports requires an investment in the community.
Start-up costs, along with the need to ensure that people continue to
receive care while new community options come on line, have hampered
states' ability to ensure that resources follow individuals into the
community. Until community services are up and running, Medicaid and other
sources of reimbursement cannot be tapped. Accordingly, states may need to
make a direct appropriation of their general funds for this purpose.
But far from meeting these obligations, states have been reducing
spending on mental health services over past years. For example:
- State only appropriations for mental health services are
significantly lower today (adjusted for inflation and growth in
population) than they were in 1955, when most people with mental illness
were warehoused in state institutions.
(8)
Given that institutions provided little in the way of real treatment
at that time, it would be expected that state expenditures for mental
health would have grown, as new and effective approaches to care and
supports were developed.
- State appropriations for mental health have lost ground, by 7
percent, between 1990 and 1997. This is true for nearly every state, as
shown in the comparison of states adjusted for inflation in the table
below.
- State appropriations for mental health have been falling in relation
to other state spending. Spending on mental health has grown more slowly
than (1) total state-government spending, (2) state-government spending
on health and welfare and (3) spending on corrections.
(9) During the 1990s, state mental health spending grew by 33
percent, but total state spending grew 56 percent, spending on health
and welfare services grew by 50 percent and spending on corrections, by
68 percent.
The overall change in real purchasing power for state mental health
appropriations between 1955 and 1997 is shown in the chart below. While
other funds supplement these state expenditures (for example, the federal
Medicaid match and the federal mental health block grant), these falling
numbers represent a reduction of states' own efforts over the years.
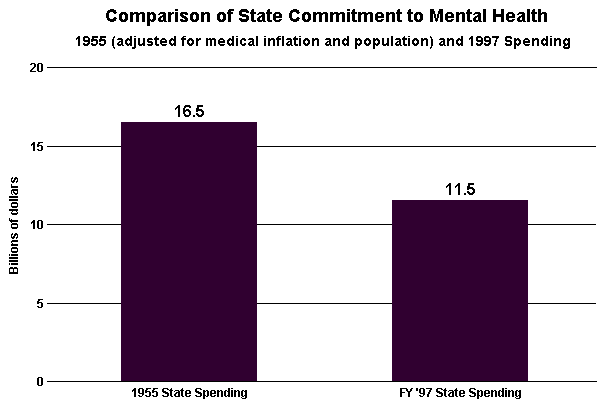 [D] [D]
(Source: Bazelon Center for Mental Health Law, Under Court Order:
What the Community Integration Mandate Means for People with Mental
Illnesses)
Accordingly, it would hardly be a fundamental alteration in programming
for states to increase their appropriations for community mental health
services in order to comply with the Supreme Court's ruling in
Olmstead. Investment in community services has the potential to
bring about long-term savings by enhancing states' ability to tap into
federal dollars, making increased investment in developing community
services and supports even more important.
Chapter 3
Impact on Children and Youth
Crisis Focus
As is well documented elsewhere,
(10) children with emotional disturbance experience significant
gaps between the systems of care designed to serve their needs and to
support them with their families and in the community. Due to the stresses
of poverty, children and youth from low-income families are
disproportionately represented among young people diagnosed with emotional
disturbance. While this labeling theoretically entitles children to a wide
range of services and supports, these are often not delivered. In
addition, the labeling itself may serve to reinforce a view of these
children as dysfunctional, and relegate them to segregated settings.
Public policy must seek to reduce this stigma while delivering supports
and services (including naturalistic supports, such as mentoring,
after-school programs and improved housing).
The Substance Abuse and Mental Health Services Administration (SAMHSA)
estimates that 20 percent of all children from birth to 17 years of age
suffer from a diagnosable mental, emotional or behavioral illness.
(11)
According to SAMHSA, approximately 7 million children had a diagnosable
mental disorder in 1997. Between children and adolescents aged 9 to 17,
SAMHSA estimates 2.1-4.1 million (five to 13 percent) have a mental or
emotional disorder that seriously impairs their functioning in day-to-day
activities.
America's youth is the human resource capital of America's future. The
value of these human resources is incalculable. We cannot define or put a
value on the loss incurred when today's children and youth with emotional
disturbance are damaged in their formative years by systems' failures to
provide needed mental health care and/or special educational services. For
example, children who lack these services often cannot utilize the free
and appropriate public education to which they are entitled under federal
law. Children with unrecognized or untreated emotional disabilities cannot
learn adequately at school or benefit readily from the kinds of healthy
peer and family relationships that are essential to becoming healthy and
productive adults.
Many young people with emotional disturbance are already involved in
the juvenile justice system.
(12) Rates of emotional disturbance among youth in the juvenile
justice system have been estimated at 60-70 percent. A significant
percentage of the 100,000 youth detained in correctional facilities each
year suffers from serious mental disabilities and a commensurately large
percentage suffer from addictive disorders. Seventy-five percent of the
youth in the juvenile system have conduct disorders and more than half
have co-occurring disabilities.
According to a 1999 report by Substance Abuse and Mental Health
Services Administration, when compared with adolescents having fewer or
less serious behavioral problems, adolescents with behavioral problems
such as stealing, physical aggression, or running away from home were
seven times more likely to be dependent on alcohol or illicit drugs.
While major mental illness, such as schizophrenia, is often evident
only when the individual reaches the late teens or early twenties, there
is little doubt that many other disabilities found among the adult prison
population surfaced at a much younger age--and went untreated.
The failure to identify (and treat) emotional disturbances is also
associated with the growing problem of teen suicides and/or suicide
attempts. If properly implemented, Medicaid's EPSDT screening program
should assist parents of youth with emotional disturbance and school
personnel in identifying their disabilities, providing the appropriate
treatment, and preventing suicide.
The lack of home- and community-based services has still other negative
consequences. The lack accounts for unnecessary hospitalization of
children and youth with emotional disturbance. It also contributes to
readmission. For lack of services that might ease the transition from
hospital to home, including respite services for their families, these
children cycle back and forth between hospital and the community without
ever achieving stability. In turn, unnecessary hospitalization usurps the
limited resources of state mental health budgets, thus obstructing the
provision of services that might have prevented institutionalization and
perpetuating an unproductive cycle.
If all aspects of the system--from assessment to treatment--took into
account the long-term needs of children, rather than episodic or crisis
occurrence, children's needs would be described in terms of their
underlying issues and in the context of their family and living situation
instead of mere documentation of short-term behavior or services
available. For some children, the system must be prepared to make a
commitment to serve the child for their entire childhood, with easy entry
and re-entry into the system. Outcome measures should reflect long-term
goals--such as school attendance, living at home with family or
independently, and working at a job.
Missed Opportunities for Prevention
Poor treatment by the system as a child or youth increases the
likelihood of encountering other dysfunctional systems as an adult.
Children with serious emotional disturbance have the civil right to
receive services in the most integrated setting appropriate to their
needs.
(13) They further have the human right to be raised in their
families and communities, with their individual needs guiding the service
array provided. These civil and human rights are embodied in the Americans
with Disabilities Act (ADA).
(14)
The failure to identify and treat mental disabilities between children
and youth has serious consequences, including school failure, involvement
with the justice system and other tragic outcomes. As outlined in the
Adult chapter, below, adults with mental illnesses who find themselves in
the criminal justice system are significantly more likely to have grown up
in foster care, under custody of a public agency or in an institution.
There are large discrepancies between the mental health needs of
children and youth and the services they actually receive. A recent study
found that only one in five children with emotional disturbance used any
mental health specialty services, and a majority received no mental health
services at all. This is consistent with an earlier finding by the Office
of Technology Assessment (OTA) which estimated that only 30 percent of the
7.5 million children who needed mental health treatment received it.
However, children with serious emotional disturbance often do not receive
the services to which they are entitled under the Individuals with
Disabilities Education Act (IDEA).
Individuals with Disabilities Education Act: IDEA has long been
the primary vehicle for securing mental health services and supports for
children and youth with mental, emotional or behavioral disabilities. The
Act's basic tenet is that, until age 21, children and youth are entitled
to "a free and appropriate public education." Under IDEA, children with
emotional or behavioral disabilities that interfere with their ability to
learn are entitled to special education services, including any related
mental health services and supports that enable them to benefit from their
education. Yet despite the intent of this strong federal entitlement,
parents and advocates report that children are not receiving many of the
promised and needed services. Children and youth with emotional and
behavioral disabilities are the least likely to receive the services and
supports mandated by IDEA.
The 1997 IDEA amendments mandated that school systems provide two new
services to address the needs of children and youth with behavioral
problems that interfere with their learning or the learning of those
around them. Schools must conduct "functional behavioral assessments"
(FBA) to determine the causes of undesirable behavior and develop
"positive behavioral interventions and supports" (PBIS) to address them.
According to Robert Horner, Ph.D., of the University of Oregon faculty,
"research conducted over the past 15 years has demonstrated the
effectiveness of strategies that foster positive behavior for individual
students and for entire schools. Even schools with intense poverty, a
history of violence and low student skills have demonstrated change in
school climate when effective behavioral systems have been implemented."
Despite this history of success, parents and school personnel report
that schools are not implementing the provisions of the 1997 IDEA
amendments. Some profess they don't understand the statute; others are
ignoring or actively subverting the law. In almost all cases, it is
apparent that school personnel are unaware of how effective (and
relatively inexpensive) these interventions can be.
EPSDT and Medicaid: Medicaid-eligible children should also
benefit from the early screening required under the Medicaid's Early
Periodic Screening, Diagnosis and Treatment (EPSDT) mandate and a
generally broader array of services in state Medicaid plans than is
available in the private sector. Under EPSDT, all states must screen
Medicaid-eligible children, diagnose any conditions found through a screen
and then furnish appropriate medically necessary treatment to "correct or
ameliorate defects and physical and mental illness and conditions
discovered by the screening services."
(15)
Children and youth up to age 21 have a broader entitlement than adults
who qualify for Medicaid. For adults, some services are mandatory, but
some need only be provided at a state's option. A state will list its
"optional" services in its Medicaid plan, but must make available to
children all services listed in federal Medicaid law "whether or not such
services are covered under the state plan."
(16) Few states have good tools to identify children with mental
health needs and most fail to monitor providers or health plans to ensure
that children receive behavioral health screens.
Medicaid's EPSDT program, especially when used in conjunction with
IDEA, is the ideal vehicle for meeting the comprehensive mental health
needs of children and youth. The program requires that states conduct
regularly scheduled examinations (screens) of all Medicaid-eligible
children and youth under age 22 to identify physical and mental health
problems. If a problem is detected and diagnosed, treatment must include
any federally-authorized Medicaid service, whether or not the service is
covered under the state plan. If problems are suspected, an
"inter-periodic" screen is also required so the child need not wait for
the next regularly scheduled checkup.
Child mental health services under Medicaid have undergone considerable
change over the past decade. For many years, states had included more
comprehensive mental health benefits for adults than for children and
youth. After the enactment of legislation requiring coverage of all
Medicaid-covered services for children through the Early Periodic
Screening Diagnosis and Treatment (EPSDT) mandate in 1990, states began
revising their rules and expanding coverage of child mental health
services.
Shortly after these revisions began to occur, states also began to move
the Medicaid population in need of mental health care into managed care,
generally into separate "carved-out" specialized managed behavioral health
care plans. By 1998, 54 percent of Medicaid beneficiaries were enrolled in
managed care programs.
(17)
(Health Care Financing Administration, 1998). Due to the rapid
expansion of covered services early in the 1990s and the subsequent
introduction of managed care, it is pertinent to question whether children
and youth actually receive these community-based services and to determine
the patterns of service use. Key stakeholders continue to cite the lack of
attention to the special needs of children and youth as the most serious
problem with the public mental health system.
(18)
By offering waivers and options Medicaid law also affords states other
policy choices that could expand access to mental health services. The
Home-and Community-based Waiver allows states to provide alternatives to
hospitalization to children with disabilities, including children and
youth with emotional disturbance. The waiver allows states to provide
various community support services, but only three states have availed
themselves of this waiver for children with emotional disturbance.
Significantly, however, a recent study indicates that the Medicaid
home-and community-based waiver is effective in reducing the incidence of
custody relinquishment and institutional placement in the three states
where they are in use.
(19)
However, Medicaid does not cover all low-income and other children and
adolescents who have no access to mental health treatment. Moreover, while
the array of covered services is fairly broad, some home- and
community-based services are still excluded from coverage under many state
Medicaid programs.
Denial and Inaccessibility of Services
Despite the IDEA and EPSDT entitlements, children and youth in many
states fall through the cracks of the public systems of care. This happens
even in states like California, with well-developed local government
infrastructure:
"Despite the integrity of individual programs-and even with the
extraordinary contributions of so many individual
professionals-incremental efforts add up to less than the sum of their
parts. The programs often fall short of providing the right services, in
the right way, to the right children at the right time. Year after year,
new commitments--even with additional funding--fail to achieve the goals
so desperately desired."
(20)
Services are often denied not out of malice, but because of the lack of
coordination among systems of care and complexity of funding
arrangements:
"Funding is restricted by complex rules that encourage communities to
forsake those in the path of danger and focus only on those children who
are physically bruised and emotionally broken."
(21)
Moreover, the criteria that youth must meet before they can receive
services can easily be interpreted to deny services.
(22) In practice, many states do not have specific definitions
of all covered services, so it is likely that many Medicaid-eligible
children receive neither the mental health screens nor the mental health
treatment to which they are entitled by EPSDT. The shortage of
knowledgeable legal advocates virtually ensures that the rights of many
children to EPSDT services will not be enforced.
Access to services is limited due to lack of insurance coverage for
mental health services and inadequate access to the special education and
related mental health services for which children and youth are eligible
through IDEA. For example, ten million children and youth lack health
insurance and many more are under-insured for mental health treatment and
exhaust their benefits. An estimated 30 percent (3 million) of those 10
million are eligible for Medicaid, but their families are unaware that
they qualify.
(23)
As states have sought to "do more with less," they have also sought out
managed care approaches to limiting Medicaid expenditures. Instead of
bridging the gap between child-serving agencies, however, states' shift of
Medicaid to managed care has stranded even more children with serious
mental health needs.
(24)
Tragic Consequences for Children, Youth and Society
Custody Relinquishment: Due to lack of community-based services
and/or special education services, families of children with emotional
disturbance are often faced with the heart-wrenching choice of not
receiving adequate mental health services for their children or
relinquishing custody of their children in order to qualify for Medicaid.
Child mental health advocates and professionals have recognized the issue
of custody relinquishment for many years.
(25)
Requiring families to give up custody:
- traumatizes both children and parents;
- limits family involvement in key decisions about their children's
mental health, health and educational needs;
- undermines family integrity;
- unnecessarily burdens public agencies with children who are neither
abandoned; nor neglected, but whose families need services and support
to raise them at home; and
- penalizes families for the state's failure to develop adequate
services and supports.
Requiring families to relinquish custody to the child welfare system in
order to obtain essential mental health services and supports for their
children wastes public funds and destroys families.
Inadequate funding of mental health services and support for children
and their families is the major reason families turn to the child welfare
system for help. Private insurance plans often have limits on mental
health benefits that can be quickly exhausted if the child has serious
mental health needs. In addition, many private plans do not provide the
home and community-based services and supports that are needed to keep
children at home. When their personal funds run out, families are forced
to turn to the child welfare system.
Even families whose children are eligible for Medicaid face custody
relinquishment. Although many of the needed services are covered, states
fail to adequately define their rehabilitation services, to educate
providers on how to bill for those services, or to make sure that Medicaid
recipients know the array of services to which a child is entitled. When
parents then turn to the child welfare agency, the agency often
requires--as a nonnegotiable condition for obtaining those
services--relinquishment of custody to the state or county. In large part,
this is driven by the child welfare agencies' mistaken belief that custody
is required in order to draw federal matching funds under the Social
Security Act.
Educational System/Special Education/Discipline: Due to the
stresses of poverty, children and youth from low-income families are
disproportionately represented in the young population with emotional
disturbance. The inequities of the neglect of these children by schools
and the public mental health system are further compounded by racial
discrimination.
The failure to provide early screening and mental health services has
meant that as many as 35 percent of students entering school are
considered to be at high risk for social and academic failure.
(27) Once in school, the failure or refusal to provide IDEA
services results in much greater drop out rates for children and youth
with emotional disturbance.
(28) This has led researchers to recommend a new approach to
screening, and to identifying a child's strengths rather than deficits.
In perhaps the classic attempt to blame the victim, school districts
that have failed or refused to provide preventive services under IDEA has
also led, inexorably, to treating children with emotional disturbance as
"discipline problems." In a series of attempts to amend the IDEA over the
past three years, Congress has increasingly expanded the authority of
school districts to exclude such children and youth from mainstream
classrooms.
The techniques for supporting children with emotional
disturbance--known broadly as "positive behavioral supports"--in school
are well documented.
(29) The use of punishment to correct behavior comes with
negative consequences such as negative attitudes on the part of students
toward school and school staff (which leads to increased antisocial acts
and behavior problems). Punishment of children with emotional disturbance
is strongly correlated with dropping out of school.
(31)
Foster care: The child protective services and foster care
system in the United States grew out of efforts by early religious and
charitable organizations to serve orphans and "rescue" children and youth
from abusive or neglectful families. Today's federally supported foster
care system was created under the Social Security Act of 1935 as a
last-resort attempt to protect children at risk of serious harm at home.
The law obligated states to assume temporary custody of children whose
parents were unable or unwilling to care for them.
By the early 1990s almost half a million children were in the custody
of state child welfare systems and the U.S. Department of Health and Human
Services estimated that at least one of every 10 babies born in poor urban
areas in the '90s would be placed in foster care.
(32)
Children with emotional or behavioral disabilities made
up 40 percent of the child welfare population and few resources were
available for any type of treatment or support services.
(33) The steady increase in foster care placements is very
troubling. Most children are deeply traumatized when they are separated
from their families. Even when their family environment has been dangerous
or unhealthy, studies have shown that a child often experiences separation
from a primary care giver as a threat to survival.
(34)
Family disintegration and allegations of abuse are the most frequent
reasons that children are placed in foster care, and these reasons are
often rooted in the inability to get mental health services and support
for parents and/or children. These findings are documented more fully in
the Custody Relinquishment section, above, and are considered further in
the Adult chapter, below.
According to the Annie E. Casey Foundation, every year 25,000 young
people in foster care turn 18 and leave foster care. This means that young
people in state-supervised programs must leave foster care whether or not
they have the skills to maintain an apartment, seek and hold a job, or
balance a checkbook. Too many 18-year-olds emerge without having had a
stable foster-care environment or adequate mental-health services or a
quality education. According to one recent study, 12 to 18 months after
they left foster care, half of those who left were unemployed and a third
were receiving public assistance. Clearly, youths who "age-out" of foster
care are among the most vulnerable and the most at risk.
Juvenile Justice: Each year, more than one million youth come in
contact with the juvenile justice system and more than 100,000 are placed
in some type of correctional facility. Studies have consistently found the
rate of mental and emotional disabilities higher among the juvenile
justice population than among youth in the general population. As many as
60-75 percent of incarcerated youth have a mental health disorder; 20
percent have a severe disorder and 50 percent have substance abuse
problems.
(35)
The most common mental disabilities are conduct disorder, depression,
attention deficit/hyperactivity, learning disabilities and posttraumatic
stress.
(36) According to a 1999 survey conducted by the National Mental
Health Association (NMHA) and the GAINS Center, mental health problems
typically are not identified until children are involved with the juvenile
justice system, if at all.
Although African-American youth age 10 to 17 constitute only 15 percent
of their age group in the U.S. population, they account for 26 percent of
juvenile arrests, 32 percent of delinquency referrals to juvenile court,
41 percent of juveniles detained in delinquency cases, 46 percent of
juveniles in corrections institutions, and 52 percent of juveniles
transferred to adult criminal court after judicial hearings. In 1996,
secure detention was nearly twice as likely for cases involving black
youth as for cases involving whites, even after controlling for
offenses.
(37)
Many youngsters have committed minor, nonviolent offenses or status
offenses. The increase in their incarceration rates is a result of
multiple systemic problems, including inadequate mental health services
for children and more punitive state laws regarding juvenile offenders.
These nonviolent offenders are better served by a system of closely
supervised community-based services, including prevention, early
identification and intervention, assessment, outpatient treatment,
home-based services, wraparound services, family support groups, day
treatment, residential treatment, crisis services and inpatient
hospitalization.
Intensive work with families at the early stages of their children's
behavioral problems can also strengthen their ability to care for their
children at home. These services, which can prevent children from both
committing delinquent offenses and from re-offending, are most effective
when planned and integrated at the local level with other services
provided by schools, child welfare agencies and community organizations.
More than one in three youths who enter correctional facilities "have
previously received special education services, a considerably higher
percentage of youths with disabilities than is found in public elementary
and secondary schools."
(38)
Many children with emotional disturbance end up in detention facilities
as a result of incidents at school and/or because they fail to receive
special education and related mental health services. In addition, many
juveniles are released from detention facilities without appropriate
discharge services, and end up being re-incarcerated.
Young people with emotional disturbance are punished for the failure of
systems designed to protect them. Because schools fail to identify and
serve youth with emotional disturbance, these children miss out on much or
all of the "free and appropriate public education" to which they are
entitled under the federal Individuals with Disabilities Education Act
(IDEA), even though IDEA funds services for such children.
(39)
Although IDEA requires educational plans to be in place prior to a
young person's release from juvenile detention, and a well-designed and
implemented plan, coupled with connections to the services provided under
Medicaid, can mean the difference between a successful transition to home
and community or a repeat of the negative cycle that landed the juvenile
in detention in the first place, few states implement this requirement.
Thus, juvenile offenders with emotional disturbance frequently fail to
reconnect with the education system upon their release.
Without the appropriate intervention, students whose behavior could and
should be addressed in school are ending up in juvenile detention. Each
year over 100,000 youth are detained in correctional facilities. These
institutions have been called the "de facto" psychiatric institutions for
adolescents with mental health problems because they substitute
incarceration for needed treatment. A recent survey by the Pittsburgh
Post-Gazette found that 80 percent or more of the residents of
Pennsylvania's juvenile detention centers had a diagnosable psychiatric
problem. Arkansas and New Mexico reported that 90 percent of their
juvenile detainees were on psychotropic medication.
Effects of Welfare Reform: In the implementation of welfare
reform, policy makers have to date focused rather narrowly on the needs of
the adult recipients. In particular, reform efforts have concentrated on
recipients who are relatively well-positioned to enter the workforce, that
is, who do not have evident disabilities or special needs. States have
declared remarkable success in their initial efforts to reduce welfare
rolls, moving off welfare large numbers of individuals and capitalizing on
the current demand for workers. Now, states are beginning to face some
unanticipated consequences of return-to-work policies particularly on
adults with significant problems (such as those who have mental health and
substance abuse issues) and on parents whose children have special needs.
States are facing the reality that there is a residual population of
welfare recipients whose capacities to work are challenged by these
problems.
What might easily be overlooked in the debate on welfare reform is that
the children of welfare recipients--both those who have already been
counted as "successes" and those remaining on welfare due to special
needs--may, themselves, have significant problems. Recipients who have
successfully returned to work may have marginal work skills and find
themselves in low-level jobs. When they have children with serious
emotional disturbance, they may be confronted with parental demands that
pull them away from already-precarious work situations. For example,
school systems are often ill prepared to deal with special-needs children
and seek to exclude them from the classroom. Child care centers are often
not prepared to handle children with significant behavioral problems and
these children may be expelled, creating significant job-related problems
for the parent.
Those welfare recipients who have not yet entered the workforce
includes significant numbers of individuals with significant problems of
their own, such as depression, post-traumatic stress disorder, and
chemical dependency. These problems among parents have been identified as
risk factors for emotional disturbance among their children. The movement
of these adults into the workforce, which is already a formidable goal,
may pose new problems for their high-risk children. For example, children
with serious emotional disturbance who have been reliant on parental care
and supervision within the home may, for the first time, be entering child
care arrangements outside of the home. These settings must be prepared to
offer special approaches appropriate to the needs of these children. In
addition, it is likely that the workplace success of recipients who are
already struggling to overcome their own problems will be compromised by
the added stress of disruptions in their children's functioning.
This array of factors suggests that the special needs of children do
not simply coexist with welfare reform; parental return-to-work has both
an effect upon these children and is affected by these children.
However, few policies thus far have considered the interaction of welfare
reform and recipients' children with serious emotional disturbance. Most
states have not worked to ensure that the needs of these children are
addressed. As the policy and legislative focus comes to be redirected to
the hardest to serve welfare recipients (which may well include a
significant number of parents of children with special needs), the well
being of children will increasingly come to be an issue.
Psychiatric Hospitalization and "Residential Care":
Traditionally, the mental health services available to children with
emotional disturbance have tended to fall at two ends of a continuum: 1)
treatment in a residential facility and 2) individual, usually once-a-week
therapy. Yet youth with emotional disturbance need one or more of a broad
spectrum of therapeutic modalities between these two poles. These include
ongoing intensive services in their home community and school.
Additionally, their families need support services, education and training
on how to best handle the youngster and his or her problems.
In many cases, the lack of home-and community-based mental health
services results in unnecessary institutionalization. Deprived of
services, the condition of many children and youth with emotional
disturbance worsens and reaches crisis proportions, leaving commitment to
a residential treatment facility as the only option. Though residential
treatment centers lack studies supporting their effectiveness, this
treatment--which serves a small percentage of youth --consumes one-fourth
the outlay on child mental health.
(40)
Referrals to residential treatment facilities--often
unnecessary--remove the child far from home and community; sometimes out
of the county or even the state for extended periods of time. Moreover,
after leaving the hospital, the lack of transitional services and/or
intensive in-home services and supports frequently result in children and
adolescents cycling from home to hospital and back again without ever
achieving stability.
However, effective home- and community-based services--such as in-home
services, behavioral aides, intensive case management, day treatment,
family support and respite care, parent education and training, and
after-school and summer camp programs--do exist. Of these services, the
Surgeon General's report found home-based services and therapeutic foster
care to have the most convincing evidence of effectiveness.
(41)
These services are furnished in partnership between professionals and
families, are clinically and fiscally flexible, and individually tailored
for each child and family, providing whatever intensity of service is
needed. Home- and community-based services build on strengths and normal
development needs rather than just focusing on problems, and provide
continuity of care. They strive to be culturally competent and involve the
family in the child's care. Evaluations of these community-based services
have found them to be highly effective, less costly than the alternative
residential services and much preferred by families.
(42)
Chapter 4
Impact on Adults
Crisis Focus
Every year, youth who have been ill-served by mental health, education
and foster care "age out" of those systems and become adults, without the
explicit entitlements to mental health and other care they had as youth.
Despite the inevitability of this process, the adult mental health system
does little to anticipate their arrival, and invests little in programs of
prevention. Like the youth-serving systems examined in the last chapter,
the adult systems devote very few resources to people until they reach the
point of crisis.
For adults, neglect or poor treatment by the mental health system
increases the likelihood an adult with mental illness will encounter other
more coercive and crisis-oriented systems, like law enforcement,
corrections, institutionalization and emergency rooms. Absent the services
and supports they need in the community, people with serious mental
illness become caught up in the criminal justice system. Ironically, these
individuals are often discharged from jails and prisons into the community
with little or no planning for treatment. Lacking treatment, their lives
become a revolving door of arrest, incarceration, release and rearrest.
With coordination among these systems almost totally lacking,
individuals and families living with mental illnesses are faced with a
mental health system that swings between the extremes of abject neglect
and unwanted intervention, never quite providing the appropriate level of
services to sustain them in the community:
- Underfunded systems ration care to those "most in need," almost
guaranteeing that people will be denied services and supports until they
are in crisis;
- Without preventive services and supports, most individuals and
families living with mental illnesses have difficulty attaining economic
self-sufficiency, and become more dependent on inadequate "safety net"
programs like Supplemental Security Income disability and welfare
payments;
- Once in crisis, the mental health, criminal justice and correctional
systems are primed to respond with coercive measures which tend to
undermine the principles of self-determination and consumer direction,
and make it harder to achieve recovery and economic self-sufficiency;
and
- Crisis-driven services (and monitoring of coercive measures) are
dramatically more expensive; they drain resources away from voluntary,
preventive services in the community, resulting in long waiting lists
and further deterioration of people in need.
By now, it is beyond debate that it is fiscally more prudent to address
mental health needs before they reach the point of crisis.
(43)
But the extraordinarily low priority placed on mental health services,
and the "Balkanization" of state budgets virtually ensures that agencies
will continue to seek out ways to push "bothersome" clients onto the rolls
of other public agencies.
Missed Opportunities for Prevention
Big Investments in Big Hospitals and Precious Little for
Community-Based Services: Historically, mental health systems have
devoted a large share of their resources to sustaining large psychiatric
hospitals in urban centers or in rural areas. One of the most
straightforward ways to finance community services for individuals who
would otherwise be needlessly institutionalized is to redirect
institutional funds to community services.
Since 1955, states have been reducing the capacity of their state
psychiatric institutions. However, until quite recently they accomplished
this by reducing the size of the hospitals, not by closing them down. More
recently, states have begun to close entire institutions, freeing up
considerable state resources that can be redirected to support community
living. For example, more state psychiatric hospitals were closed in the
first half of the 1990s than in the 1970s and 1980s combined.
(44)
Since 1990, a total of 40 such hospitals have been closed.
Recent experience in Indiana demonstrates how such an approach can
produce both positive outcomes for individuals and savings for the
state.
(45)
Indiana closed a hospital that was housing individuals with serious
mental illness who had a mean length of stay of over eight years. After
the hospital closed, most went to some form of 24-hour care or monitoring
in the community and were served by programs providing intensive levels of
service. The state also provided three years of special funding to local
community programs specifically to ease the transition for these
individuals. This funding, redirected from hospital spending, allowed
communities to meet the needs of dischargees without squeezing them into
existing treatment slots or adding to already over strained community
programs.
The individuals benefitted from services in more integrated settings
and showed positive outcomes, such as improved functioning and quality of
life. Savings for the state were significant. Per-person costs went from
$68,400 for a year's hospital care to $40,600 for those placed in the
community. However, some individuals were placed in alternative
institutions (such as a nursing homes, which do not represent community
integration), whose costs were a little higher. As a result, the overall
average cost for the year following closure was $55,417 per person
discharged. Still, this represented a savings of 19 percent of funds
expended to maintain these individuals in the state hospital.
Counter to this trend, and to the clear mandate of the Supreme Court's
Olmstead decision, some states have dug in their heels, and have
attempted to rebuild large state institutions, while starving
community-based mental health care. One such example is Laguna Honda
Hospital, a 1,200-bed skilled nursing facility owned and operated by the
City and County of San Francisco. Three fourths of the facility's annual
reimbursement comes from Medicaid and Medicare. The city is proposing to
build another huge public facility and an assisted living building on the
same grounds as the current nursing home. The citizens of San Francisco
passed a bond referendum allowing the city to spend up to $299 million to
create a facility or facilities to replace Laguna Honda. Such an
expenditure would foreclose the development of the community-care options
required under Olmstead.
(46)
Denial And Inaccessibility of Services
Medicaid is a principal source of funding for the health and mental
health services that states offer in the community to public-sector
consumers released from institutional settings under the Olmstead
mandate. The Social Security Act allows states to waive traditional
Medicaid rules to set up systems of managed care for Medicaid enrollees.
States began using the waivers to offer medical services through managed
care. By now, many have expanded their waivers to include (mental health
and addiction treatment for some or all of the Medicaid population.
This shift of Medicaid into managed care arrangements is beginning to
blur the borders that have distinguished public and private sectors. At
first, the populations with more extensive service needs largely remained
in fee-for-service Medicaid programs; however, states are now planning
ways to refine these systems to eliminate the inefficiencies of
overlapping, cumbersome bureaucracies. They are also beginning to evaluate
their expenditures in terms of the clinical outcomes they are purchasing.
Whether directly, through managed care contracts with commercial insurance
companies, or through states' application of business practices to
fee-for-service systems, the experiences of the private market are being
transported to the public sector and the respective systems are moving
closer together. In communities, individuals and families encounter both
considerable overlap and significant gaps in services, with no one
organizational structure that can resolve these defects. The trend appears
to be increasing with the introduction of managed care plans into Medicaid
mental health service delivery.
Community Mental Health is Closed When it Should be Open: As a
consequence of underfunding, poor resource allocation and the (not
infrequent) desire to shift the cost of hard-to-serve clients to other
public systems, the community mental health system in most states is only
"open" from 9 a.m. to 5 p.m. Unlike other public systems, like emergency
rooms, law enforcement and corrections, which are "open" 24 hours per day,
seven days per week, the mental health system is often "closed" (except
for hospital-based services) during evenings and weekends, when many
people with mental illnesses experience the greatest need. During those
times, when adults with mental illnesses come to the attention of the
police, they are processed through the justice system (or taken to an
emergency room for psychiatric evaluation), rather than being diverted to
the less-costly, more appropriate community-based mental health service
system that should be meeting their needs.
Geographic Inaccessibility: Even if they have some sort of
insurance coverage, many adults with mental illnesses who live in rural
areas lack effective access to the mental health services and supports
they need because they simply live too far from providers, who are
typically centered in urban and suburban areas. The advent of managed care
in the Medicaid and public mental health systems over the past ten years
has further diminished the number of providers willing to serve rural
clients.
Language and Cultural Barriers: Most state mental health systems
still lack the ability to serve people of color and language minorities in
their own traditions and their own language. The Surgeon General recently
reported "striking disparities" in mental health care for racial and
ethnic minorities, and that these disparities "impose a greater disability
burden on minorities," and that people from diverse cultures collectively
experience a greater disability burden from mental illness than do whites.
This burden is directly attributable to the fact that people from diverse
cultures systemically receive less care and poorer quality of care, rather
than from their illnesses being inherently more severe or prevalent in the
community.
(47)
TRAGIC CONSEQUENCES FOR ADULTS AND FOR SOCIETY
Homelessness: On any given day, approximately 150,000 people
with severe mental illnesses are homeless, living on the streets or in
public shelters. Homelessness is not a symptom of mental illness. It is an
artifact of mental health systems that do not link consumers to accessible
housing and do not offer needed supports and services, or that operate
residential programs experienced by consumers of mental health care as
coercive. Homelessness among people with serious mental illnesses
underlies many of the problems that spill over from the mental health
system, including the problem of criminalization. Yet the successes
reported by many local programs demonstrate that most homeless people with
mental illnesses can live with stability in their communities if they
receive a combination of sustained outreach, case management, health and
mental health services, housing and employment assistance.
(48)
Criminalization of Mental Illnesses: Jails are becoming
America's new mental hospitals. As a result, jail facilities are faced
with a role they were neither designed nor staffed to assume. Between
600,000 and one million men and women jailed each year have a mental
illness. This is thought to be eight times the number admitted to
psychiatric hospitals. Many of these people are arrested for non-violent
misdemeanors, others for "crimes of survival" such as stealing food,
loitering, or trespassing. Still others are detained in "mercy arrests" by
police officers who find the public mental health system unresponsive and
the process of accessing its emergency services cumbersome.
As many as 16 percent of all jail inmates have a severe mental illness,
according to the U.S. Department of Justice. Many were arrested for
reasons related to their unmet needs for mental health or addiction
treatment and for housing. Many people with mental illnesses are homeless
and frequently arrested for "esthetic" or "quality of life" misdemeanors
that result from their lack of access to mental health services and that
police routinely ignore when committed by others.
Predominantly, prisoners with mental disabilities are poor and people
of color. Along with details about the plight of other major racial and
ethnic minority groups, a report released August 26, 2001, by the U.S.
Surgeon General, entitled Mental Health: Culture, Race and
Ethnicity, indicates that disproportionate numbers of African
Americans are represented in the most vulnerable segments of the
population--people who are homeless, incarcerated, in the child welfare
system, victims of trauma--all populations with increased risks for mental
disabilities.
People with mental illnesses, with mental retardation, and with
associated substance abuse (hereinafter "people with mental disabilities")
are increasingly brought into the criminal justice system. They are
arrested for various minor offenses--many times for "crimes of survival"
as they struggle to live on the streets--and incarcerated in jails and
prisons where their treatment needs are not met. Typically, these are
offenses people who do not have mental disabilities either would not
commit or which prompt a warning...not an arrest. Often, people with
mental disabilities are living in circumstances so characterized by
neglect that police and others in the community may even view these
arrests as acts of "mercy."
Instead of punitive actions, these individuals need assistance.
However, failures in service systems and the lack of collaboration between
mental health, mental retardation, substance abuse, and criminal justice
systems prevent them from receiving adequate supports and care. This is
especially true for individuals who are homeless, whose mental illness is
particularly hard to treat, and those with co-occurring substance
abuse.
In addition to being greater in number, inmates with mental illnesses
tend to have a history of more significant problems when compared with
other inmates. Many lead chaotic lives. Inmates with a mental illness were
less likely to be employed in the month before the arrest; 37.7 percent in
federal prisons were unemployed, compared with 27.5 percent of inmates who
did not have a diagnosis of mental illness. Inmates with a mental illness
are more likely to reflect one or more of the factors that put people at
risk, such as:
- growing up in foster care;
- living with a substance-abusing parent;
- or being physically or sexually abused;
- More likely to have been homeless;
- More likely to be unemployed at the time of arrest;
(49)
- More likely to be under the influence of drugs or alcohol at the
time of the arrest;
(50)
- More likely to grow up in foster care, agency or institution;
(51)
- More likely to have been physically or sexually abused while growing
up;
(52) and/or
- More likely to grow up with a parent who abused alcohol.
(53)
Once incarcerated, these men and women are even less likely to receive
adequate treatment than when they were at liberty--both because the
criminal justice system lacks the capacity to deliver comprehensive mental
health services and because punitive jail settings are the antithesis of a
therapeutic environment. In all likelihood, the number of incarcerated
people with disabilities has increased, given the extensive publicity
accorded to violent acts by people with mental illnesses, however rare,
along with the increased public cynicism about deinstitutionalization, the
diminished tolerance of abnormal behavior and the expanding use of police
tactics such as "mercy arrests."
(54)
While some jails and prisons provide mental health services, the
emphasis should not be on improving these services in a coercive
anti-therapeutic environment. Rather, investment should be made in
diversion. It should extricate people with mental illnesses from the
revolving door of re-arrest, they must be provided with discharge planning
to help them obtain public benefits and link them to community treatment.
Yet nationally, only one third of inmates with mental illnesses receive
discharge planning services.
When released from jail or prison, inmates with mental illnesses seldom
receive the assistance they need for successful re-entry into the
community.
(55)
Without adequate discharge planning prior to release, they have no
access to medication and other needed mental health services, to housing,
or to employment or income support.
(56) Studies have shown that recidivism rates fall when
discharge planning and linkage to effective aftercare services is
provided.
Individuals sentenced to jail or prison lose their entitlement to
Medicaid and other public benefits. There is even a financial incentive
for correctional institutions that promptly report prisoners' intake to
the Federal Government. But there is no incentive to the criminal justice
system to help released prisoners reestablish or initiate such benefits.
Reinstatement involves complex paperwork and applications take months to
process--months during which many former inmates have no money for
medication or housing, much less counseling.
As is the case with discharge from psychiatric hospitals, the incidence
of recidivism among people with mental illnesses is directly related to
the quality of post-discharge treatment and supports, including housing.
The comprehensive support model pioneered for homeless people by CSH is
highly appropriate for people with mental illnesses who are returning to
the community from jails and prisons.
Rather than focus on the handful of far-from-typical violent criminals
with untreated mental illness public policy should concentrate on
diverting non-violent offenders with serious mental illness from the
criminal justice system into community-based treatment programs and
expanding those programs so as to reduce recidivism and prevent the
actions that prompt arrest. While those who have committed serious
offenses should receive mental health treatment in jail, for those who
have committed only minor offenses that are the result of or associated
with their illness, incarceration is neither cost effective, humane nor
just. By definition, a penal institution constitutes a non-therapeutic
environment. In fact, inmates with mental illness are at risk of being
victimized, sexually abused and at increased risk of suicide. (Ninety-five
percent of prison or jail suicides involve inmates with a diagnosed mental
illness.)
The problem of criminalization of people with mental illness has been
exacerbated by the failure of mental health systems to meet the needs of
people in the community after deinstitutionalization vastly reduced the
population in state psychiatric hospitals. The vision of
deinstitutionalization was to allow individuals with mental illness to be
full participants in the community. This goal is even more realistic today
than it was in the 1960s. New anti-psychotic medications, effective
community services (even for those with the most serious disabilities),and
new breakthroughs in treating co-occurring mental illness and substance
abuse, make successful community living a real possibility for the vast
majority of people with mental illness. To succeed, however, they need
access to an array of comprehensive services, from housing to intensive
community mental health services.
Although preventing incarceration must always be the goal, there will
also be a continuing need for policies and programs that can provide more
effective solutions when people with mental illness make contact with the
criminal justice system. There have been isolated attempts to address this
problem through the use of diversion programs, using the criminal justice
process to steer people with mental illness from jail and into mental
health treatment.
Diversion programs offer a variety of approaches, some of which have
been criticized for offering no more than a choice "between forced
medication or jail." Although diversion programs have been determined
effective from a criminal justice perspective--i.e., their use reduces the
number of inmates with mental illness--their efficacy has not been studied
from a mental health or civil rights perspective. We need to know whether
people with mental illness who are diverted from jails are receiving
mental health treatment that allows them to participate in community life
and avoid further contact with the criminal justice system and whether
their civil rights have been respected during the process.
Mental Health Courts
As a response to the growing number of people with mental illnesses
being confined to jail or prison, a number of local jurisdictions have
developed mental health courts. These specialty courts are modeled on drug
courts, and purport to focus on "therapeutic jurisprudence" rather than
punishment. In 2000, Congress passed legislation to provide limited
funding for mental health courts in 50 jurisdictions.
Advocates, however, are wary of the courts:
Mental health courts are, to many people, an appealing response to
criminalization. But the mental health courts that exist so far, with
very few exceptions, accept only people charged with non-violent
low-level offenses. While these courts help some people get services,
they do nothing to help mental health consumers facing prison or lengthy
jail sentences, and they do not reduce criminalization. If mental health
courts increase the "price" of minor offenses, as some undoubtedly do,
their effect is actually to expand criminalization, a phenomenon known
as "net-widening."
(57)
This "net-widening" is of concern because police officers may arrest
people whom they would have otherwise warned, told to "move on", or
ignored in an effort to secure them services via the mental health court.
Mental health courts may also result in people with mental illness
receiving more severe sanctions for petty criminal offenses than they
would have received through the regular court system. They may spend more
time in jail or other secure confinement; they may find themselves under
judicial supervision for a longer period of time, and they may have to
plead guilty to charges that might otherwise have been dismissed.
Moreover, they may not be adequately counseled by their lawyers as to
these potential risks, and judges and court personnel may be giving
inaccurate information concerning these risks.
Poverty/Unemployment: Improvements in treatment and advances in
community-based rehabilitation services mean that more people with serious
mental illnesses are able to work.
Unfortunately, the unemployment rate for people with mental illness
hovers at 85 percent, higher than for any other disability group. Factors
such as stigma and public misperception of mental illnesses only partially
account for this situation. Many people can and do recover from mental
illness. A variety of specialized services such as supported employment,
transitional employment and psychosocial rehabilitation enable people with
mental disabilities to work and have a satisfying and rewarding career.
Several federal agencies provide vocational rehabilitation services for
people with disabilities: the state-federal public vocational
rehabilitation system, the Social Security Administration and the
Department of Labor. These federal programs work cooperatively with state
and private rehabilitation providers to increase employment among people
with disabilities. Recent federal legislation includes provisions to
facilitate work for those who receive disability
benefits by allowing easy re-entry into rehabilitation programs if
there is a reoccurrence of symptoms and by creating a voucher program to
allow consumers to go to the provider of their choice.
The federal Vocational Rehabilitation (VR) program provides funds to
states for assisting individuals with disabilities to work. Unfortunately,
state VR programs focus primarily on individuals with less serious
disabilities. People with severe mental illnesses, in particular, do not
fare well in these systems, because they frequently require intensive
services over longer periods of time to obtain and maintain
employment.
Moreover, considerable VR resources are spent on
eligibility-determinations and administrative functions, while inadequate
resources go to direct services. Months or even years may pass between the
time an individual with a severe mental illness applies for VR services
and the time that services actually begin.
While the recently enacted Ticket to Work and Work Incentives
Improvement Act of 1999 theoretically enhances the ability of a person
with a psychiatric disability to find work without losing income and
Medicaid benefits, the new law is very complicated, and has not led to
significant new job opportunities.
Involuntary Outpatient Commitment
In many states, the abject neglect of the needs of people with
psychiatric disabilities and the predictable deterioration that will be
experienced by some has led to a call for more coercive practices, like
involuntary outpatient commitment (IOC). IOC is a legal strategy that
utilizes court orders and other means to force individuals with
psychiatric disabilities to participate in mandatory treatment, merely
because someone else has made a judgement that they would benefit from
psychiatric treatment. An individual can be forced into treatment despite
the fact that no crime has been committed and notwithstanding that he/she
does not meet the requirements for inpatient commitment (i.e., that the
person is a clear and present danger to self and/or others).
When a court issues a civil commitment order, requiring an individual
to submit involuntarily to treatment for a serious mental illness, the
person has historically been confined to inpatient treatment in a public
hospital. Today there is new interest in IOC, linked to media reports of
violent acts by individuals with diagnoses of serious mental illnesses
and, according to state advocates and mental health consumers, fueled by a
sophisticated public relations campaign by the Treatment Advocacy Center.
Increasingly, the providers of mental health services to individuals thus
committed are private-sector programs, including psychiatric clinics and
group homes.
Private providers--whose cooperation is required to implement these
statutes--are split on IOC. A good many, particularly social workers, case
workers and others working on a person-to-person level, believe that the
requisite reporting on their clients harms the therapeutic relationship
and that the clients'--not coerced--but voluntary participation is
essential to the healing process.
The National Council on Disability has previously expressed its
concerns about such coercion, and reiterates them here:
Mental health treatment should be about healing, not punishment.
Accordingly, the use of aversive treatments, including physical and
chemical restraints, seclusion, and similar techniques that restrict
freedom of movement, should be banned. Also, public policy should move
toward the elimination of electro-convulsive therapy and psycho surgery as
unproven and inherently inhumane procedures. Effective humane alternatives
to these techniques exist now and should be promoted.
(58)
Involuntary outpatient commitment is a very costly effort to the
individual, to the mental health system, to the criminal justice system,
and to society that holds no promise of the avoidance of violence in our
society, nor of recovery for the individual. It diverts badly needed
funding away from effective community-based mental health services,
especially those founded upon the recovery vision.
Like so-called "mercy arrests" that bring people with mental illnesses
into the criminal justice/correctional system, IOC is used far too often
to compensate for gaps in community services that would otherwise engage
mental health consumers on a voluntary basis.
Psychiatric Hospitalization
When all else fails, the mental health system retains the ability to
petition for the involuntary civil commitment of a person whose mental
illness makes him or her a threat to self or others. In the civil
commitment context, federal courts have said that the Due Process Clause
requires a balancing of the individual's interest in liberty against the
state's interest in providing care and treatment to the individual in
order to protect the public (police power) or to protect the individual
(parens patriae).
(59)
As outlined above, however, the crisis focus of mental health services
virtually ensures that "all else" will fail, and the system will
have to rely upon hospitalization.
Chapter 5
Impact on Seniors
Crisis Focus
Like younger adults, seniors with psychiatric disabilities and limited
incomes rely upon public mental health services and supports they may need
to live successfully in the community. They rely upon many of the same
providers as do younger adults, although the possibility of physical
disabilities or frailty in this population make it more likely that they
may be living in nursing homes, assisted living facilities or other
similar settings that may not adequately provide mental health services
and supports. In those instances, many seniors either go entirely without
such services, accept the marginal services that may be available in those
settings, or depend upon the limited services and supports funded by
Medicare or Medicaid and delivered by community-based providers.
(60)
Mental health care for older Americans is no better than for the
younger cohorts considered in earlier chapters. According to the American
Association of Geriatric Psychiatry, nursing homes currently are charged
each year with the care of 1.5 million older Americans. More than half
suffer from some sort of cognitive impairment and as many as 80 percent
have a diagnosable psychiatric disorder. Despite the high prevalence of
people with mental disabilities in nursing homes, according to the Surgeon
General's report, "these settings generally are ill equipped to meet their
needs."
(61)
Likewise, in the Journal of General Psychiatry, mental health
experts from around the country warn that "(a) national crisis in
geriatric mental health care is emerging. The present research
infrastructure, healthcare financing, pool of mental health care personnel
with appropriate geriatric training, and the mental health care delivery
system are extremely inadequate to meet the challenges posed by the
expected increase in the number of elderly with mental illness as well as
an anticipated increase in late-onset mental illness as more people live
longer."
Significant challenges to the mental health of older adults relate less
to our clinical capacities than they do to older adults not having access
to services known to be effective. For example, notwithstanding the high
prevalence of depression among older adults, the Surgeon General reports
that only 11 percent of older adults are receiving adequate treatment and
55 percent receive no treatment whatsoever. Indeed, very few of the 15-25
percent of older adults over 65 who--according to U.S. Census Bureau
estimates--have a mental illness, receive treatment. Most community
surveys suggest that 1 percent or fewer older adults in their community
receive psychiatric care. They remain underserved by mental health
providers, as shown by the following data:
- Only 4 percent of community mental health center patients are over
65.
- Fewer than 4 percent of the patients seen by private practitioners
are older adults.
- Less than 1.5 percent of all community-based mental health care goes
to older adults.
A number of factors contribute to the lack of community-based services
for older adults with mental illnesses. Many elders in nursing homes whose
chronic physical ailments do not require institutionalization (e.g.,
diabetes) are confined to these settings because they have a serious
mental illness--although effective treatment for both the former and the
latter is routinely administered in the community.
Additionally, to a degree, the low utilization rates for
community-based care reflect older cohorts' sense of shame around mental
health problems and their aversion to seeking help. But they also are
testimony to stagnant public systems that have long traditions of
neglecting older adults' mental health needs that afford older adults low
priority and that, rather than providing rehabilitation, relegate older
adults to custodial care services. The consequences of the unavailability
or inaccessibility of appropriate services to older adults with mental
illness include additional and unnecessary disability, needless dependency
and vulnerability to institutional segregation.
Missed Opportunities for Prevention
Older adults are the most rapidly growing segment of our population.
Due in part to increasing life expectancy, people over 65 are expected to
grow in number from 20 million in 1970 to 69.4 million by 2030,
outnumbering people between 30 and 44. Additionally, there is evidence
that the number of older adults with mental illness will also increase in
terms of both numbers and in the percentage of the total population that
those numbers represent. Thus, the number of older adults with mental
illness is projected to swell from about four million in 1970 to 15
million in 2030.
Denial and Inaccessibility of Services
The December 1999 Report of the U.S. Surgeon General--the first
of 51 such reports to focus on mental health--devotes a chapter
specifically to older adults and mental health. While acknowledging the
capacity for sound mental health among older adults, the report notes "a
substantial proportion of the population 55 and older--almost 20 percent
of this age group--experience specific mental disabilities that are not
part of normal aging. Unrecognized or untreated, depression, Alzheimer's
disease, alcohol and drug misuse and abuse, anxiety, late-life
schizophrenia and other conditions can be severely impairing, even fatal;
in the United States, the rate of suicide, which is frequently a
consequence of depression, is highest among older adults relative to all
other age groups (Hoyer et al., 1999)."
Yet there are effective interventions for most mental disabilities
experienced by older persons (for example, depression and anxiety and many
mental health problems such as bereavement). Further, the Surgeon
General's report asserts that "treating older adults with mental health
disorders accrues other benefits to overall health by improving the
interest and ability of individuals to care for themselves and follow
their primary care provider's directions and advice, particularly about
taking medications."
The Supreme Court's Olmstead decision has
particular significance for older adults with mental disabilities.
Arguably--more so than any other group with mental illness--older adults
have endured a long history of flagrant segregation and societal neglect,
most graphically demonstrated in the deplorable "geriatric back wards" of
state psychiatric hospitals. Despite the shift away from psychiatric
institutions and the promise of community mental health services, older
adults continue to be afforded "back ward" status, as evidenced by a
paucity of community-based mental health services, limited opportunities
for integrated housing, and service systems that emphasize custodial care
over rehabilitation. In fact, largely motivated by cost savings and
convenience rather than clinical need, substantial numbers of older adults
with mental disabilities were trans-institutionalized from state
psychiatric hospitals to nursing homes. Among other people with mental
disabilities, the pivotal Olmstead decision applies to:
- long-stay patients in psychiatric hospitals who do not need to be
there;
- individuals who frequently cycle in and out of hospitals as a result
of a lack of community services;
- residents in nursing homes who can appropriately be served in the
community;
- individuals residing in the community, but at risk of
institutionalization unless they receive appropriate care.
Like younger people with mental illnesses, seniors are at significant
risk of unnecessary institutionalization. A recent analysis of
Olmstead complaints filed with the Office of Civil Rights of the
U.S. Department of Health and Human Services reveals that 60 per cent of
the complaints have been filed by people living in nursing homes.
(62) ADA--and the integration mandate, in particular--compels
states to consider the civil rights of people with disabilities and to
determine whether their systems of care perpetuate needless segregation
and its harmful effects. As states move to comply with these legal
requirements for diverse populations of disabled individuals, aging
advocates face the challenge of ensuring that older adults are not put at
the end of the line as they compete for limited resources.
Chapter 6
Fulfilling the Promise: Concrete Steps
Toward a New Vision
For each population covered in this report, there are concrete steps
that can be taken to improve the quality and effectiveness of mental
health services and supports.
Children and Youth
ENABLING CHILDREN AND YOUTH WITH MENTAL OR EMOTIONAL DISABILITIES TO
FLOURISH IN THEIR COMMUNITIES: Children with emotional disabilities
fall through an historic gap between the various child-serving agencies in
the public sector--notably, the education, child welfare, juvenile justice
and mental health systems. Efforts to improve this situation should focus
on promoting the systems of care that have been demonstrated effective in
bridging the gap and enabling children to receive Medicaid-funded
wraparound services in their homes or in residential settings near their
families.
STATE EFFORTS TO EXPAND MEDICAID COVERAGE TO CHILDREN AND YOUTH WITH
EMOTIONAL DISTURBANCE THROUGH THE USE OF WAIVERS AND OPTIONS. Since
Congress has recently provided states with an opportunity--through the
Child Health Insurance Program--to expand Medicaid coverage to families
with incomes higher than the Medicaid eligibility ceiling, the Medicaid
entitlement can likewise be extended to more children. Studies of home-and
community-based waivers have focused primarily on the growth in the number
of waivers and the cost-effectiveness for aged individuals, individuals
with mental retardation and developmental disabilities and persons with
AIDS. Among the groups covered in the mid-1990s, individuals with mental
retardation and developmental disabilities reflected the most rapid
growth. They increased from 74,000 in 1992 to 146,000 in 1996. The Centers
for Medicare and Medicaid services is currently funding a study to
evaluate the impact on quality of life, quality of care, utilization, and
cost for individuals with mental retardation and developmental
disabilities. Few studies have examined the use of home-and
community-based waivers for children with emotional
disturbance.
PREVENTING EXCLUSION FROM SCHOOL OF CHILDREN WITH EMOTIONAL
DISTURBANCE: Identify and disseminate a range of services that
progressive school systems have provided through IDEA and under court and
administrative rulings, identifying for state policymakers and advocates
the maximum range of community-based services for children with emotional
disturbance that can be furnished under the IDEA, and enforce the
requirement to conduct functional behavioral assessments and to provide
positive behavioral supports.
PREVENTING CUSTODY RELINQUISHMENT THROUGH ACCESS TO CHILD MENTAL
HEALTH SERVICES: The Family Opportunity Act would create a new state
option to allow states to expand Medicaid coverage to children with
disabilities up to age 18, who would be eligible for SSI disability
benefits except for family income or resources. Any family with a child
whose disability meets SSI criteria and whose income does not exceed 300
percent of the poverty level could be covered under Medicaid if the state
chooses this option. The bill also creates a time limited demonstration
program to extend Medicaid coverage to children who have a disability that
would become severe enough to qualify under SSI if they are left to
deteriorate without health care. The demonstration will provide useful
information on the cost effectiveness of early health care intervention
for children with potentially severe disabilities.
The Family Opportunity Act would add residential treatment centers to
the waiver statute and thus allow states to provide waivers to families
seeking home and community based services instead of more restrictive care
in such centers.
(63)
EXTENDING MEDICAID AND OTHER BENEFITS TO YOUTH AGING OUT OF FOSTER
CARE: The vast majority of young people in the foster care system are
there because they have experienced some form of childhood maltreatment.
Research reveals that negative childhood experiences, especially abuse and
neglect, can adversely affect adult health and mental health. Adults with
aversive childhood experiences are also more likely to be depressed,
attempt suicide, have unintended pregnancies, and have personality
disorders. Substance abuse problems and alcoholism are also correlated
with negative childhood experiences. Extension of Medicaid benefits will
help address the needs of these youths. Health care benefits will allow
young people to receive treatment for health or mental health problems
before the problems become severe.
FEDERAL LEGISLATION ON AMENDING INSURANCE LAWS TO END PRACTICES THAT
HAVE THE EFFECT OF DISCRIMINATING AGAINST PERSONS WITH MENTAL ILLNESS:
Legislation should be drafted to address the unequal access to mental
health care that is prevalent in all aspects of the United States health
care system, including private insurance, public insurance, and programs
designed to bridge the gaps between the private and public health
insurance sectors.
DOCUMENT HOW EXISTING ENTITLEMENT PROGRAMS CAN BE USED TO PREVENT
CONTACT WITH THE JUVENILE JUSTICE SYSTEM AND TO DIVERT CHILDREN AND YOUTH
FROM JUVENILE JUSTICE. In its 2000 report, From Privileges to
Rights, NCD called upon Federal, state, and local governments,
including education, health care, social services, juvenile justice, and
civil rights enforcement agencies to work together to reduce the placement
of children and young adults with disabilities, particularly those labeled
with emotional disturbance, in correctional facilities and other
segregated settings. These placements are often harmful, inconsistent with
the federally-protected right to a free and appropriate public education,
and unnecessary if timely, coordinated, family-centered supports and
services are made available in mainstream settings.
Advocates have begun to document how existing entitlements to family
supports and community-based intensive mental health treatment can prevent
children's behavior from deteriorating to the point of warranting
incarceration. The National Mental Health Association and the GAINS Center
have recommended that communities: (1) formalize screening and assessment
for mental health and substance abuse for youth at all points of contact
of the juvenile justice system; (2) provide the full range of mental
health and substance abuse services and supports to youth, and cease the
piece meal, stop gap approach that currently exists; and (3) establish a
coordinating body or task force that focuses on this population of
youth.
(64)
PROTECTING BENEFITS UNDER WELFARE REFORM FOR PARENTS WITH MENTAL
ILLNESSES AND PARENTS WHOSE CHILDREN HAVE EMOTIONAL DISABILITIES: As
Congress considers reauthorization of the 1996 "welfare reform" law, it
has the opportunity to strengthen the entitlement to cash payments and
Medicaid benefits for poor families in which a parent or child has
significant mental health issues which prevent a head of household from
returning to work.
Adults and Seniors
ADA/OLMSTEAD OFFER SOLUTIONS: ENDING ISOLATION AND
SEGREGATION
While a state is not obliged to assume an "undue burden" in its pursuit
of integrated services for people with serious mental illnesses, nothing
in Olmstead requires community placements to be "cost-neutral."
Indeed, the entire tenor of the decision is to the contrary. The court
recognizes that needless institutionalization is a wrong that the ADA was
designed to redress. It is clear that an accommodation under the ADA can
be reasonable even if it imposes costs.
The court did not identify when it would be "too costly" for a state to
provide services in the community. (The issue was not before the court.)
Instead, the court identified relevant factors, the most significant being
the resources available to the state to fund community services. While the
existing community services system constitutes one available resource, the
court made clear that other resources must also be counted. The
Olmstead decision anticipates the reallocation of resources to fund
community placements.
In evaluating what resources are available to finance community
placements, states need to look both at services that are currently funded
and at how community services might be funded if the state took action to
maximize its budget. These "available resources" can include resources
that the state could obtain by aggressively seeking additional funds--from
the legislature, by restructuring its Medicaid program or through similar
strategies.
PROVIDE A LEGALLY ENFORCEABLE RIGHT TO MENTAL HEALTH SERVICES AND
SUPPORTS: By providing a right to services and supports "in sufficient
amount, duration, scope and quality to support recovery, community
integration and economic self-sufficiency," a law could transcend the
age-old debate about inadequate funding.
For example, the Bazelon Center for Mental Health Law has drafted a
proposal which would provide a legally enforceable right to
recovery-oriented mental health services and supports, and will be working
with advocates in several states around the country to press for its
adoption.
(65) This proposal seeks to reshape the debate about mental
health system reform. This initiative is driven by a growing consensus
among many stakeholders that traces a host of social ills affecting adults
with serious mental illnesses--homelessness, vagrancy, criminalization and
so-called "mercy arrests", unemployment and needless dependency on public
systems--to a single cause. That cause is the inadequacy of the public
mental health system, which does little more than provide crisis services
and fails to meaningfully address the long-term rehabilitative needs of
the population it serves. It is clear that the absence of an entitlement
to appropriate, timely mental health services has increased the number of
people with mental illnesses in crisis.
MAXIMIZE THE AVAILABILITY OF MENTAL HEALTH SERVICES AND SUPPORTS
PROVIDED THROUGH CONSUMER-DIRECTED ORGANIZATIONS: People labeled with
psychiatric disabilities should have a major role in the direction and
control of programs and services designed for their benefit. This central
role must be played by people labeled with psychiatric disabilities
themselves, and should not be confused with the roles that family members,
professional advocates, and others often play when "consumer" input is
sought. For the past decade, the Federal Government has provided funding
and logistical support for three consumer-run technical assistance
centers. These centers have helped to document, establish and refine
successful alternative approaches to the provision of mental health
services and supports through the use of other people who have experienced
mental illnesses. The Federal Government should increase incentives to
state mental health systems to adopt such models and to expand their use.
ENSURE THAT ALL MENTAL HEALTH SERVICES AND SUPPORTS ARE VOLUNTARY IN
NATURE, AND NOT CONTINGENT ON COMPLIANCE WITH MEDICATION OR TREATMENT
PLANS: NCD reaffirms its commitment to the principles enunciated in
its 2000 report, From Privileges to Rights: "Eligibility for
services in the community should never be contingent on participation in
treatment programs. People labeled with psychiatric disabilities should be
able to select from a menu of independently available services and
programs, including mental health services, housing, vocational training,
and job placement, and should be free to reject any service or program.
Moreover, in part in response to the Supreme Court's decision in
Olmstead v. L. C., state and federal governments should work with
people labeled with psychiatric disabilities and others receiving
publicly-funded care in institutions to expand culturally appropriate
home- and community-based supports so that people are able to leave
institutional care and, if they choose, access an effective, flexible,
consumer/survivor-driven system of supports and services in the
community."
FEDERAL LEGISLATION ON AMENDING INSURANCE LAWS TO END PRACTICES THAT
HAVE THE EFFECT OF DISCRIMINATING AGAINST PERSONS WITH MENTAL ILLNESS:
Legislation should be enacted to address the unequal access to mental
health care that is prevalent in all aspects of the United States health
care system, including private insurance, public insurance, and programs
designed to bridge the gaps between the private and public health
insurance sectors.
A longstanding history of discrimination and recrimination has led to
policies which systemically deny needed health care to millions of
Americans with severe mental health needs. People with mental illness have
been alternatively thought of as possessed by evil spirits, lazy,
responsible for their own illness, and infantile. In the past, individuals
with mental health impairments were locked in institutions. Today, they
are locked in jails and prisons because they are unable to access the care
that they need.
The underlying stigma surrounding mental illness has led to systemic
inequality in all health care delivery. For example, the private sector
refuses to insure individuals with a history of any mental health
treatment, when they will insure an individual with more severe physical
health care needs. In addition, caps on doctors' visits, hospital days and
other services are placed on mental health care, but not on physical
health care.
Private insurance, however, is evenhanded between physical and mental
health care in its denial of long term care to individuals with ongoing
health care needs. To address this gap in private coverage, the Medicaid
program has developed waivers and options which provide health care
coverage for a more intensive package of services to individuals who would
not usually qualify for publicly funded health care by virtue of their
income. These "bridge" programs, however, do not meet the needs of
individuals with mental health impairments. For example, the waiver and
option statutory language does not include residential treatment
facilities, which are where most children with serious emotional
disturbance languish for long periods. As a result, only 3 states have
received waivers for children with serious emotional disturbance, where 50
states have waivers for children with developmental disabilities. In
addition, almost half the states with an option program for children do
not serve any children with a primary diagnosis of serious emotional
disturbance. States fail to serve children with mental health needs even
though the federal statutory language does not exclude them in any way and
makes the option available to any child with a disability.
Finally, Medicare and Medicaid, the public health safety net, provide
unequal services to individuals with mental health needs. Medicare
reimburses a much lower percentage of mental health care costs than
physical health care costs. Medicaid also fails to meet the needs of
individuals with mental illness. States do not include needed mental
health services in their Medicaid plans. When individuals enter jails and
prisons because of a lack of services in the community, their Medicaid
coverage is immediately terminated in every state, despite federal law
which allows states to suspend coverage and thus, facilitate reentry into
the community upon discharge. Under the Early Periodic Screening Diagnosis
and Treatment program mandating necessary services for children, few
states provide an adequate mental health screening tool for children and
studies indicate that large percentages of children are not screened at
all. Federal law does not require states to report on mental health
screening rates or ensure that an adequate mental health screening tool is
used.
All three means of health care coverage--public, private and bridge
programs--create barriers to the receipt of mental health care. These
barriers have led to the current national crisis, with individuals with
severe mental health needs increasingly relying on emergency room care,
prisons, and jails to fill the gap. Congress must act to remove those
impediments and redress the longstanding discrimination against
individuals with mental illness which can only be explained by ignorance
and stigma.
NCD reiterates the concern expressed in From Privileges to
Rights that to assure that parity laws do not make it easier to force
people into accepting "treatments" they do not want, it is critical that
these laws define parity only in terms of voluntary treatments and
services.
IMPROVE VOCATIONAL REHABILITATION (VR) SERVICES: Individuals
with severe mental illnesses would like the option to seek VR services
directly from private programs with proven track records in providing
effective services, bypassing ineffective, VR bureaucracies. A variety of
approaches could be considered, such as providing vouchers that would
permit individuals to purchase services from a range of programs meeting
quality standards.
The Ticket to Work and Work Incentives Improvement Act is a step in
this direction because it authorizes the Social Security Administration to
provide vouchers that allow consumers on SSI and SSDI to select their own
training and placement provider. The ticket pays private providers over a
60-month period, so long as the individual stays off cash benefits,
thereby creating strong incentives for providers to offer ongoing,
flexible supports and services designed to keep individuals in jobs.
However, to benefit from this program individuals must have been receiving
federal disability benefits and must be able to work full time. Other
individuals with disabilities could also benefit from psychiatric
rehabilitation services, yet there is no program for them under the
Rehabilitation Act.
ESTABLISHING A RIGHT TO MENTAL HEALTH DISCHARGE PLANNING PRIOR TO
RELEASE FROM JAIL OR PRISON
A national strategy is needed to stop the revolving door for inmates
with mental illnesses.
Establishing a right to discharge planning under federal law would have
a far greater impact than a series of state decisions, however valuable.
Establishing a right to discharge planning is only one step toward ending
the harmful, often cyclic, incarceration of people with mental illnesses.
Efforts are also underway to reconnect former inmates with federal
benefit programs like Supplemental Security Income and Medicaid, so that
they have some income, health care and medication benefits to help them
transition successfully back to the community.
(66)
PROVIDE ADEQUATE FUNDING FOR ENFORCEMENT OF THE ADA, IDEA, FAIR
HOUSING ACT AND OTHER CIVIL RIGHTS LAWS AFFECTING PEOPLE WITH PSYCHIATRIC
DISABILITIES: Government civil rights enforcement agencies and
publicly-funded advocacy organizations should work more closely together
and with adequate funding to implement effectively critical existing laws
like the Americans with Disabilities Act, Fair Housing Act, Civil Rights
of Institutionalized Persons Act, Protection and Advocacy for Individuals
with Mental Illness Act, and Individuals with Disabilities Education Act,
giving people labeled with psychiatric disabilities a central role in
setting the priorities for enforcement and implementation of these
laws.
CHAPTER 7
An Inter-Generational Vision for Effective Mental
Health Services and Supports
As outlined in Chapters 3, 4, and 5, the fragmentation of the public
mental health system has had a devastating impact on children, youth,
adults and seniors with mental illnesses. And the disconnects between
systems of care serving each of these populations have exacerbated these
impacts further. Children and youth with severe emotional disturbance who
do not get early screening and preventive services are more likely to find
themselves poor and dependent on an adult mental health system that does
not serve their needs. Unserved adults are likely to become unserved
seniors.
Fundamental reform will require new thinking about how systems of care
can invest--over a lifetime, if necessary--in adequate mental health
services and supports that will allow children to live successfully with
their families in the community, and will allow adults and seniors to seek
recovery from the effects of mental illnesses and to achieve economic
self-sufficiency.
Expanding the Resource Base
While there is no question that additional resources are needed to
address America's mental health needs, policy makers must be educated
about the "penny-wise and pound-foolish" manner in which mental health
services and supports are currently delivered. As outlined in Chapters 1
and 2, the inability of the public mental health system to deliver
preventive services and supports often leads people with mental illnesses
into more restrictive and less humane settings, such as jails and prisons,
homeless shelters and state hospitals. But that approach is substantially
more expensive overall.
The Supreme Court's Olmstead decision also demonstrates how
funds can be recaptured from unnecessary institutionalization. Recently,
there has been renewed emphasis on reducing the use of long-term hospital
care, especially for people with the most severe mental illnesses.
(67)
Improved community treatments, such as psychiatric rehabilitation,
consumer peer support and intensive case management programs, have become
more widely available. Helping to fuel this movement are continuing
concerns over the relative ineffectiveness and therapeutic limitations of
inpatient care, including the dependencies it creates, and the fact that
community care is generally no more expensive than institutional care.
Ironically, as a society, we may be paying much more for an ineffective
patchwork of programs than we would for a comprehensive set of preventive
services and supports. The cost of emergency hospitalization in a private
hospital in an urban setting can be over $1000/day. So-called "residential
treatment programs" can cost as much as $750/day. At $350/day, even state
psychiatric hospital care is quite expensive. People with mental illnesses
who find themselves in state prisons or local jails cost taxpayers over
$100/day, and homeless shelters impose a similar tax burden. By
comparison, proven models like supportive housing
(68) cost much less, while providing many more opportunities for
community integration.
The challenge here is to convince federal and state policymakers to
adopt a longer budgetary view, and one that captures all of the costs of
neglecting the public mental health system and the pressing needs of its
consumers. A few communities have attempted such dramatic restructuring,
with promising results. For instance, Vermont has secured a "Medicaid 1115
Waiver" to allow it to provide flexible and comprehensive services and
supports through its Community Rehabilitation and Treatment (CRT) program,
and has devoted state funding to provide housing and other services not
reimbursable under Medicaid. As a consequence, each of the 3,200 adults in
the CRT program has access to a broad range of supports that are tailored
to his or her specific needs.
(69)
Similarly, in Los Angeles, the Village Integrated Services Agency is a
comprehensive program for people with serious mental illnesses (clients
are called members at the Village). The Village offers an array of options
for members which supports individualized services in all quality of life
areas (i.e. employment, housing, social, substance abuse, etc.). Staff
focus on encouraging members' free choice of any menu option at any
time.
(70)
Federal resources to support the expansion of community services
required under Olmstead are available to states from several
sources, including Medicaid's optional services for adults:
- targeted case management and rehabilitation;
- Medicaid coverage for services furnished in small community
residential programs of fewer than 16 beds;
- Medicaid's array of comprehensive community services for children,
mandated through the Early and Periodic Screening, Diagnosis and
Treatment requirement of the law;
- Medicaid Home- and Community-Based Care Services Waiver; and
- expanding Medicaid eligibility through various options and waivers
of federal rules--home- and community-based service waivers (Section
1915(c) of the Social Security Act), research and demonstration waivers
(Section 1115), the option to cover people who are medically needy under
Medicaid, and coverage of children with emotional disabilities under the
"Katie Beckett" option (Section 1902(e)(3)).
Despite the availability of such funding, many states have elected not
to apply.
(71)
States also have the authority to allow certain health care providers
to "presumptively" enroll children in Medicaid who appear to be eligible
based on their age and family income. This can be done based on the
family's declaration that its income is below the state's Medicaid
income-eligibility guidelines. The child can then be provisionally
enrolled in Medicaid and begin to receive services, while a full Medicaid
application with the necessary information is prepared and submitted (this
must be done by the end of the following month). States that fail to cover
all eligible children, adults and seniors under Medicaid are losing the
opportunity to secure federal matching funds for the home- and
community-based services these people need.
Improving Access and Reducing Barriers to Securing Supports,
Services, Treatment
Because cost of services is the most significant problem facing poor
people with mental illnesses, expanding Medicaid eligibility and
reimbursable services--concrete steps available to every state--are the
most significant steps that can be taken to improve access to mental
health services and supports for children, adults and seniors. The federal
Medicaid program provides matching funds for such efforts, but many states
experiencing budget shortfalls are loath to increase their own
contributions, even when these leverage federal funds at very favorable
levels.
The Surgeon General has outlined a program of action for improving
access and reducing barriers for people of color and language minorities.
These focus on coordinating early intervention and care to "vulnerable,
high-need groups.... It is not enough to deliver effective mental health
treatments: Mental health and substance abuse treatments must be
incorporated into effective service delivery systems, which include
supported housing, supported employment, and other social services."
(72)
Barriers caused by geography are more difficult to address. Many rural
areas simply lack the infrastructure to provide even basic mental health
services and supports to any population. Rural practitioners are focusing
more attention on integrating mental health services into traditional
family practices, and on the use of telemedicine.
(73)
Promoting Recovery
Today, unfortunately, the services and supports available to most
people with serious mental illnesses are neither sufficient nor
recovery-oriented. They are designed primarily to reduce the most obvious
symptoms, minimizing the need for expensive hospitalization but promising
little more. Driven at least in part by low expectations, these stopgap
services rarely aim at promoting independence, gainful employment and
fulfilling relationships--goals we all seek. And even these services are
in extremely short supply, depriving many consumers of the only help,
however inadequate, that might enable them to avoid unemployment,
homelessness or contact with the criminal justice system.
But we have to avoid the temptation of defining success as the mere
reduction of people with mental illnesses who are unemployed, homeless or
in jail. Clearly, people who have been diagnosed with mental illnesses
seek more than just abatement of their symptoms. They also want and
deserve an opportunity to succeed in the community. What is most needed is
a new vision that promotes the goal of recovery from mental illness,
rather than the view that mental illnesses are lifelong afflictions that
need to be managed. Just as the national "welfare reform" debate pushed
the country to conceive of a new way to move families from dependence to
independence, the mental health community needs to rethink how resources
can be allocated to promote independence of people with mental illness
diagnoses.
Conclusion
Thirty years ago, the nation decried conditions on the back wards of
state psychiatric hospitals, which were often referred to as "snake pits,"
in which people with psychiatric disabilities were "warehoused" rather
than helped to recover. Since then, through years of litigation, research
and experience, public mental health systems have developed innovative
models to support people with psychiatric disabilities in integrated
settings in the community. But lack of visionary leadership and inadequate
funding have prevented these models from "going to scale" in order to
serve more people.
Instead, many public mental health systems are stuck in neutral gear,
content that people with psychiatric disabilities will be "maintained" in
the community, rather than supported in their recovery and helped on the
road to economic self-sufficiency. In other words, the aspirations of many
public mental health systems--as measured by actual programmatic and
financial commitments rather than rhetoric--has not, for most people with
psychiatric disabilities, changed much in 30 years. Instead of being
warehoused on back wards of hospitals, many people with psychiatric
disabilities today are warehoused in homeless shelters, jails and prisons
and other isolated and segregated settings throughout our communities.
What is most needed now is a dramatically new vision of what people
with psychiatric disabilities can achieve, if given the supports they need
to succeed. That vision must start with the premise that recovery is
possible and ought to be seen as an objective for every person with a
psychiatric disability. The vision must also incorporate the principles of
the ADA and the Supreme Court's Olmstead decision, which declared
that the unnecessary institutionalization of people with disabilities is a
form of discrimination and that each state has an affirmative duty to move
people with psychiatric disabilities out of isolated and segregated
programs (whether in hospitals or in the community) and into settings
where they are truly integrated into community life. A final component of
this new vision will require a commitment to fund effective supports and
services and to fund enforcement of the rights guaranteed under the ADA,
IDEA, Medicaid and other federal statutes.
The Federal Government can play an important role in establishing
funding and other incentives for state mental health systems to adopt new
models that support this vision and that are consistent with
Olmstead and President Bush's New Freedom Initiative.
Appendix
Mission of the National Council on Disability
Overview and Purpose
The National Council on Disability (NCD) is an independent federal
agency with 15 members appointed by the President of the United States and
confirmed by the US Senate. The overall purpose of NCD is to promote
policies, programs, practices, and procedures that guarantee equal
opportunity for all individuals with disabilities, regardless of the
nature or significance of the disability, and to empower individuals with
disabilities to achieve economic self-sufficiency, independent living, and
inclusion and integration into all aspects of society.
Specific Duties
The current statutory mandate of NCD includes the following:
- Reviewing and evaluating, on a continuing basis, policies, programs,
practices, and procedures concerning individuals with disabilities
conducted or assisted by federal departments and agencies, including
programs established or assisted under the Rehabilitation Act of 1973,
as amended, or under the Developmental Disabilities Assistance and Bill
of Rights Act, as well as all statutes and regulations pertaining to
federal programs that assist such individuals with disabilities, in
order to assess the effectiveness of such policies, programs, practices,
procedures, statutes, and regulations in meeting the needs of
individuals with disabilities.
- Reviewing and evaluating, on a continuing basis, new and emerging
disability policy issues affecting individuals with disabilities at the
federal, state, and local levels and in the private sector, including
the need for and coordination of adult services, access to personal
assistance services, school reform efforts, and the impact of such
efforts on individuals with disabilities, access to health care, and
policies that act as disincentives for individuals to seek and retain
employment.
- Making recommendations to the President, Congress, the Secretary of
Education, the director of the National Institute on Disability and
Rehabilitation Research, and other officials of federal agencies about
ways to better promote equal opportunity, economic self-sufficiency,
independent living, and inclusion and integration into all aspects of
society for Americans with disabilities.
- Providing Congress, on a continuing basis, with advice,
recommendations, legislative proposals, and any additional information
that NCD or Congress deems appropriate.
- Gathering information about the implementation, effectiveness, and
impact of the Americans with Disabilities Act of 1990 (42 U.S.C. 12101
et seq.).
- Advising the President, Congress, the commissioner of the
Rehabilitation Services Administration, the Assistant Secretary for
Special Education and Rehabilitative Services within the Department of
Education, and the director of the National Institute on Disability and
Rehabilitation Research on the development of the programs to be carried
out under the Rehabilitation Act of 1973, as amended.
- Providing advice to the commissioner of the Rehabilitation Services
Administration with respect to the policies and conduct of the
administration.
- Making recommendations to the director of the National Institute on
Disability and Rehabilitation Research on ways to improve research,
service, administration, and the collection, dissemination, and
implementation of research findings affecting persons with disabilities.
- Providing advice regarding priorities for the activities of the
Interagency Disability Coordinating Council and reviewing the
recommendations of this council for legislative and administrative
changes to ensure that such recommendations are consistent with NCD's
purpose of promoting the full integration, independence, and
productivity of individuals with disabilities.
- Preparing and submitting to the President and Congress an annual
report titled National Disability Policy: A Progress Report.
International
In 1995, NCD was designated by the Department of State to be the U.S.
government's official contact point for disability issues. Specifically,
NCD interacts with the Special Rapporteur of the United Nations Commission
for Social Development on disability matters.
Consumers Served and Current Activities
Although many government agencies deal with issues and programs
affecting people with disabilities, NCD is the only federal agency charged
with addressing, analyzing, and making recommendations on issues of public
policy that affect people with disabilities regardless of age, disability
type, perceived employment potential, economic need, specific functional
ability, veteran status, or other individual circumstance. NCD recognizes
its unique opportunity to facilitate independent living, community
integration, and employment opportunities for people with disabilities by
ensuring an informed and coordinated approach to addressing the concerns
of people with disabilities and eliminating barriers to their active
participation in community and family life.
NCD plays a major role in developing disability policy in America. In
fact, NCD originally proposed what eventually became the Americans with
Disabilities Act. NCD's present list of key issues includes improving
personal assistance services, promoting health care reform, including
students with disabilities in high-quality programs in typical
neighborhood schools, promoting equal employment and community housing
opportunities, monitoring the implementation of the ADA, improving
assistive technology, and ensuring that those persons with disabilities
who are members of diverse cultures fully participate in society.
Statutory History
NCD was initially established in 1978 as an advisory board within the
Department of Education (P.L. 95-602). The Rehabilitation Act Amendments
of 1984 (P.L. 98-221) transformed NCD into an independent agency.
NOTES
1. Vermont has secured a "Medicaid 1115 Waiver" to
allow it to provide flexible and comprehensive services and supports
through its Community Rehabilitation and Treatment (CRT) program, and has
devoted state funding to provide housing and other services not
reimbursable under Medicaid. As a consequence, each of the 3,200 adults in
the CRT program has access to a broad range of supports that are tailored
to his or her specific needs. See Department of Developmental & Mental
Health Services, DESCRIPTION OF PROGRAMS AND SERVICES, at http://www.state.vt.us/dmh/
2. The term "public mental health system" refers to
the system(s) of care in a state that serves individuals and families that
are poor. The public mental health system provides more than half of all
funding for mental health services in America. While for health care,
private insurance is a major payer, the private system contributes only 46
percent for mental health, and its role is shrinking. See Health Care Plan
Design and Cost Trends: 1988 through 1997, The Hay Group, Washington, D.C.
1998. This paper focuses solely on the public systems charged with
providing mental health care and supports to poor people.
3. 3 See, e.g., Bazelon Center
for Mental Health Law, Disintegrating Systems: The State of States'
Public Mental Health Systems (December 2001); Abigail Trafford,
"Second Opinion: Writing Off Depression," The Washington Post,
Tuesday, January 1, 2002; Page HE01.
4. See, e.g.,Criminal Justice / Mental Health
Consensus Project, at http://www.consensusproject.org/
. "Life on the Outside," All Things Considered, May 30, 2000,
available at http://www.npr.org/ramfiles/atc/20000530.atc.06.rmm
(Cook County Jail is Illinois' biggest mental health facility).
5.
344 F.Supp. 387, 391 (M.D. Ala.1972), aff'd sub nom. Wyatt v.
Aderholt, 503 F.2d 1305 (5th Cir. 1974).
6. Where to Turn: Confusion in Medicaid Policies on
Screening Children for Mental Health Needs, Bazelon Center for Mental
Health Law, 1999.
7. The Center for Mental Health Services' Community
Mental Health Services Block Grant awards grants to the States to provide
mental health services to people with mental disabilities. Through the
Community Mental Health Services Block Grant, a joint Federal-State
partnership, CMHS supports existing public services and encourages the
development of creative and cost-effective systems of community-based care
for people with mental disabilities. With the current changes in the
health care delivery system, improving access to community-based systems
is especially important. See
http://www.mentalhealth.org/publications/allpubs/ KEN 95-0022/default.asp.
8. Note: State spending figure includes state and
local appropriations for mental health and excludes the federal match for
Medicaid, the federal mental health block grant, first- and third-party
payments and other non-state sources. Lutterman, T., Hirad, A. and
Poindexter, B., Funding Sources and Expenditures of State Mental Health
Agencies, Fiscal Year 1997, National Association of State Mental
Health Program Directors Research Institute, Inc. Alexandria, VA. 1999,
Table 23.
9. Id.
10. National Council on Disability, From
Privileges to Rights: People Labeled with Psychiatric Disabilities Speak
for Themselves, available at http://www.ncd.gov/newsroom/publications/privileges.html#5,,
at Chapter 5;
Bryant, E. S., Rivard, J. C., Addy, C. L., Hinkle, K. T., Cowan, T. M.,
& Wright, G. (1995). Correlates of major and minor offending among
youth with severe emotional disturbance. Journal of Emotional and
Behavioral Disorders, 3 (2), 76-84.
11. Mental Health Needs Of Many U.S. Children Going
Unmet, available at
http://www.pslgroup.com/dg/4D1FA.htm
.
12. See, e.g., Children's Defense Fund, Quick Facts:
Mental Health and Juvenile Justice (CDF), at http://www.childrensdefense.org/ss_jjfs_menthlthjj.php
13. The U.S. Supreme Court stated that individuals
have such a right unless the state can show that implementation would be a
fundamental alteration. Olmstead v. L.C., 119 S.Ct. 2176, 2188 (1999).
14. Children also have rights under the Individuals
with Disabilities Education Act (IDEA), including the right to services in
the least restrictive setting appropriate for the child. See, generally,
Bazelon Center for Mental Health Law, Olmstead Planning for Children
with Serious Emotional Disturbance: Merging System of Care Principles
with Civil Rights Law, available at http://www.bazelon.org/olmsteadchildren2.pdf
15. 42 U.S.C. §1396d(a).
16. Social Security Act, Section 1905(r)(5). See
also, Omnibus Budget Reconciliation Act, 1989, Public Law 101-239.
17. http://www.hcfa.gov/medicaid/trends98.pdf
18. Stroul, B. A., Pires, S. A., Armstrong, M. I.,
and Meyers, J. C. (1998). The impact of managed care on mental health
services for children and their families. The Future of Children:
Children and Managed Health Care, 8, 119-133.
19. Bazelon Center for Mental Health Law,
Relinquishing Custody, The Tragic Result of Failure to Meet Children's
Mental Health Needs. (Mar. 2000).
20. Little Hoover Commission, Young Hearts &
Minds: Making a Commitment to Children's Mental Health, at iv
(Report #161, October 2001), available at http://www.lhc.ca.gov/lhcdir/report161.html.
21. Id.
22. For example, to qualify for special education,
the child's mental disability must affect educational performance to a
marked degree and over a long period of time. The child must also exhibit
one or more of the following characteristics:
- an inability to learn that cannot be explained by intellectual,
sensory or health factors;
- an inability to build or maintain satisfactory interpersonal
relationships with peers and teachers;
- inappropriate types of behavior or feelings under normal
circumstances;
- a general pervasive mood of unhappiness or depression ; or
- a tendency to develop physical symptoms or fears associated with
personal or school problems.
23. The Kaiser Commission on the Future of Medicaid.
Medicaid's role for children. Medicaid Facts. Washington, DC
(1997)
24. Bazelon Center for Mental Health Law, Managed
Behavioral Health Care for Children and Youth: A Family Advocate's Guide
(1996).
25. Jane Knitzer first identified the problem in a
ground-breaking 1978 study and elaborated on it in a 1982 publication,
Unclaimed Children: the Failure of Public Responsibility to Children
and Adolescents in Need of Mental Health Services. Several later
studies confirm Knitzer's findings.
- The Research and Training Center on Family Support and Children's
Mental Health found that 25 percent of parents whose children have
emotional disturbance received suggestions that they relinquish custody.
One third of those parents receiving the suggestion gave up custody in
order to get services.
- The Commonwealth Institute for Child and Family Studies conducted a
survey of 45 states. In 28 states (62 percent), at least one agency used
custody transfer to gain access to state funding for services for
children with serious emotional and behavioral problems. Thirty-eight
(32 percent) of the responding child-serving agencies used custody
transfer to obtain funding for children's treatment
(26)
26. See n. 15, above.
- The National Alliance for the Mentally Ill surveyed parents of
children with mental and emotional disabilities and found nearly
one-fourth of them had been told by public officials that they needed to
relinquish custody to get needed services for the children.
27. Ruth Goldman, Model Mental Health Programs and
Educational Reform, American Journal of Orthopsychiatry, (1997) p.
347.
28. ABC Project, Staying in School: Strategies for
Middle School Students with Learning and Emotional Disabilities
(1995), at p. 1: "Nationally, 35 percent of students with learning
disabilities and 55 percent of students with emotional disabilities drop
out of school as compared to about 25 percent of students without
disabilities.
29. Among the most recognized of these techniques are
to:
- Personalize instruction through accommodating different learning
styles and abilities;
- Create leadership opportunities for less-popular students (such as
appointing as class helpers);
- Give student alternatives such as self-imposed time-outs, relaxation
techniques; and
- Try to eliminate conditions that lead to reactive misbehavior (such
as teasing from other students) (30)
30. UCLA Mental Health Project, B ehavior
Problems: What's a School to Do?, in Addressing Barriers to
Learning, Vol. 2, No. 2, (1997) p. 2.
31. Id. at 5.
32. "Proposal to Preserve the Family," Associated
Press, The Wenatchee (Alabama) Daily World, May 24,
1993.
33. Mental Health Law Project (now Bazelon Center for
Mental Health Law), The R. C. Case: Creating a New System of Care for
Children, 1991.
34. Firman, C., On Families, Foster Care, and the
Prawning Industry, Family Resource Coalition Report, No. 2, 1993.
35. Cocozza, J. J. (Ed.) Responding to Youth With
Mental Disorders in the Juvenile Justice System. Seattle, WA, The National
Coalition for the Mentally Ill in the Criminal Justice System, 1992.
36. Garfinkel, Lili F., Unique Challenges, Hopeful
Responses: A Handbook for Professionals Working with Youth with
Disabilities in the Juvenile Justice System, PACER Center, 1997.
37. 1999 National Report Series, Juvenile Justice
Bulletin.
38. "Special Education in Correctional Facilities,"
by the National Center on Education, Disability and Juvenile Justice
(1990). Available at http://edjj.org/Publications/pub05_01_00.html.
39. Almost always for want of special education
services, 55 percent of children with emotional disturbance drop out--more
than twice the rate of other students in the general population. Nearly 20
percent of students with emotional disturbance have been arrested,
compared with an arrest rate of nine percent for all students with
disabilities. As these children age and leave school without adequate
preparation or skills, the arrest rate climbs. Of youngsters with
emotional disturbance out of school for two years--more than a third had
been arrested. By the time they had been out of school for five years,
more than 70 percent had been arrested.
40. U.S. Department of Health and Human Services.
Mental Health: A Report of the Surgeon General (1999), at Chapter
3.
41. Id.
42. Hyde, K. L., Burchard, J. D. & Woodworth, K.
(1996). Wrapping services in an urban setting. Journal of Child and
Family Studies, 5, 67-82; Yoe, J. T., Santarcangelo, S., Atkins, M.
& Burchard, J. D. (1996). Wraparound care in Vermont: Program
development, implementation, and evaluation of a statewide system of
individualized services. Journal of Child and Family Studies, 5,
23-38.
43. 41 See, e.g., Culhane, Dennis, Comparing The
Relative Effectiveness Of Transitional vs. Supported Housing For Single
Persons With Severe Mental Disabilities Exiting Homelessness; Culhane,
Dennis, The Public Costs Of Homelessness Versus Supported Housing In
New York City: Assessing The Differential Impact On NYS Medicaid-Funded
Services, Veterans Administration Programs, The Health And Hospitals
Corporation, New York State Psychiatric Hospitals, And The New York State
Dept. Of Corrections; Corporation for Supportive Housing, The New
York/New York Agreement Cost Study: The Impact of Supportive Housing on
Services Use for Homeless Mentally Ill Individuals.
44. National Association of State Mental Health
Program Directors, State Mental Health Agency Profile System Highlights:
Closing and Reorganizing State Psychiatric Hospitals: 1996. NASMHPD,
Alexandria, VA 1997.
45. McGrew, J. H., Wright, E. R., & Pescosolido,
B. A., Closing of a state hospital: An overview and framework for a case
study. Journal of Behavioral Health Services & Research, 26:3
August 1999, 236-245.
46. There have also been recent efforts to rebuild
state psychiatric hospitals in Montana and the District of Columbia, two
jurisdictions whose community mental health systems have consistently
failed adults with mental illnesses.
47. Mental Health: Culture, Race, and Ethnicity: A
Supplement to Mental Health: A Report of the Surgeon General,
available at
http://www.surgeongeneral.gov/library/mentalhealth/cre/default.asp
48. National Coalition for the Homeless and National
Law Center on Homelessness and Poverty, Illegal to be Homeless: The
Criminalization of Homelessness in the United States (January
2002).
49. Ditton, P.M. (1999). Mental health and treatment
of inmates and probationers (Bureau of Justice Statistics, NCJ-174463,
p.5). Washington, DC: U.S. Department of Justice.
50. Id. at 7.
51. Id. at 6.
52. Id.
53. Id.
54. Inmates with mental illnesses tend to have a
history of more significant problems when compared with other inmates.
Many lead chaotic lives. The DOJ report found that: More than three
quarters of inmates with a mental illness had at least one prior prison,
jail or probation term; twenty percent of inmates were homeless in the 12
months prior to arrest, compared to 8.8 percent of other inmates; inmates
with a mental illness were less likely to be employed in the month before
the arrest; 37.7 percent in federal prisons were unemployed, compared with
27.5 percent of inmates who did not have a diagnosis of mental illness;
and inmates with a mental illness are more likely to reflect one or more
of the factors that put people at risk, such as growing up in foster care,
living with a substance-abusing parent, or being physically or sexually
abused.
55. Until litigation was commenced against it, New
York City fought the obligation to provide discharge planning in court
(Brad H. v. City of New York). The city would drop inmates released
from Rikers Island at a toll plaza in the middle of the night with $1.50
and two subway tokens. People who took medication while incarcerated are
released without a supply to carry them until they can obtain and fill a
prescription. No one ensures that they have access to public benefits such
as SSI and Medicaid, which they could use to obtain housing and mental
health treatment. Currently, however, the city has adopted a special
program where inmates diagnosed with mental illnesses who are discharged
from jail can have their medications subsidized until they are able to
re-establish Medicaid benefits.
56. A 1997 study revealed that only 20 percent of
jails nationwide engage in discharge planning. This means that most former
inmates with serious mental illnesses enter a void when they walk out of
the correctional facility. It is no wonder that the recidivism rate among
people with mental illnesses is extremely high. An effective discharge
plan is crucial to the successful re-entry into the community of an inmate
with a serious mental illness. Case managers who initiate the appropriate
process prior to the inmate's release must also be able to follow up
afterwards to make sure the individual has in fact received benefits and
services.
57. Heather Barr, Mental Health Courts: An
Advocate's Perspective, available at the "Mental Health" tab, at http://www.urbanjustice.org/publications/index.html.
58. National Council on Disability, From
Privileges to Rights: People Labeled with Psychiatric Disabilities Speak
for Themselves (January 20, 2000).
59. Vitek v. Jones, 445 U.S. 480, 491-492 (1980)("We
have recognized that for the ordinary citizen, commitment to a mental
hospital produces a massive curtailment of liberty."); Addington v. Texas,
441 U.S. 418, 425, 99 S.Ct. 1804, 1809, 60 L.Ed.2d 323 (1979)(because of
the consequences, a person with mental illness cannot be committed without
due process of law).
60. Mental health spending in Medicare, Medicaid and
other federal programs has grown more slowly than overall program
spending. Mental Health: A Report of the Surgeon General, 1999, p. 417.
Medicare law also limits the program's effectiveness in meeting the needs
of enrollees with mental and emotional disabilities. Medicare requires
beneficiaries to pay 50 percent of the cost of outpatient mental health
treatment, but only 20 percent of other outpatient services. Medicare also
provides no coverage for services that are critical for individuals with
serious mental illness (case management, psychiatric rehabilitation and
medication) and imposes a discriminatory lifetime limit of 190 days on
coverage for care in a psychiatric hospital.
61. Lombardo, N. E. (1994). Barriers to mental health
services for nursing home residents. Washington, DC: American Association
of Retired Persons Policy Institute.
62. Center for Health Care Strategies, An Analysis
of Olmstead Complaints: Implications for Policy and Long-Term Planning
(2001), available at http://www.chcs.org/publications/pdf/cas/olmsteadcomplaints.pdf.
The report does not distinguish between seniors and younger adults living
in nursing homes.
63. The bill adds the words "inpatient psychiatric
hospital services for individuals under 21" to the waiver language. This
phrase is defined in the Medicaid statute to include any facilities that
the Secretary of HHS includes in regulations. HHS has promulgated a
regulation which includes residential treatment facilities as inpatient
psychiatric services for individuals under 21, if the facilities meet
certain criteria.
64. National Mental Health Association and GAINS
Center, Justice For Juveniles: How Communities Respond To Mental Health
And Substance Abuse Needs Of Youth In The Juvenile Justice System.
Executive summary available at http://www.nmha.org/children/justjuv/execsum.cfm
65. Bazelon Center for Mental Health Law, A New
Vision of Public Mental Health: A Model Law to Provide a Right to Mental
Health Services and Supports, available at
http://www.bazelon.org/newvisionofpublichealth.html.
66. See Bazelon Center for Mental Health Law,
Finding the Key to Successful Transition from Jail to the Community: An
Explanation of Federal Medicaid and Disability Program Rules
(2001).
67. Kamis-Gould, E., Hadley, T. R., Rothbard, A. B.,
et al: A framework for evaluating the impact of state hospital closing.
Administration and Policy in Mental Health 1995: 22:497.
68. See, e.g., Sam Tsemberis and Ronda F.
Eisenberg, "Pathways to Housing: Supported Housing for
Street-Dwelling Homeless Individuals With Psychiatric
Disabilities,"
51 Psychiatric Services 487-493 (2000);
Houghton, The New York/New York Agreement Cost Study: The Impact of
Supportive Housing on Services Use for Homeless Mentally Ill
Individuals, Corporation for Supportive Housing (May 2001), available
at http://www.csh.org/NYNYSummary.pdf
.
69. See Department of Developmental & Mental
Health Services, DESCRIPTION OF PROGRAMS AND SERVICES, at http://www.state.vt.us/dmh/
70. http://www.village-isa.org/
71. See Bazelon Center for Mental Health Law,
Under Court Order: What the Community Integration Mandate Means for
People with Mental Illnesses, available at http://www.bazelon.org/undctord.pdf.
72. Mental Health: Culture, Race, And Ethnicity: A
Supplement to Mental Health: A Report of the Surgeon General (2001),
available at
http://www.surgeongeneral.gov/library/mentalhealth/cre/execsummary-6.html.
73. See National Association for Rural Mental Health
Web site, at http://www.narmh.org/.
HOME | FAQs | NEWSROOM | SITE MAP | FEDERAL
AGENCIES | RESOURCES
Last Updated: September 16,
2002 |